Nutrition and your doctor

There are certain things that doctors are great at. How to prescribe medications? Yes. How to do surgery? Yes. Nutrition and weight loss? No, definitely not. You might be a little stunned to hear that admission, coming from a highly trained medical specialist like myself. But, it all comes down to a physician’s training and what they see as their circle of competence.



Nutritional studies in med school
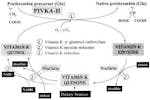


We also learned about such common everyday diseases such as scurvy (Vitamin C deficiency) and pellagra. Gums bleeding and hair follicles that are corkscrewed? Avast ye mateys. Your bloody gums are a-fouling my pirate ship, you scurvy dog. Knowledge of scurvy certainly came in handy during exams, and also for the last patient that I diagnosed with scurvy, with was, uh, never. That’s probably because I am a modern-day physician and not a pirate of the Caribbean.



The medical school, however, considers them nutrition lectures and I came through medical school with essentially zero knowledge of nutrition as most people know it. The questions that people really want to know are things like – should I eat more carbs? Less carbs? More fat? Less fat? Is sugar bad? How often should I eat? How do I lose weight? Those important health questions, apparently were not considered the purview of the medical school teachings. Medical school, with dozens of professors and academic doctors apparently were not interested enough in these questions to give much more thought to it than referring to the Canada Food Guide or the American Dietary Guidelines.
Medical school provided less training in real life nutritional questions than most health clubs or gyms. As a result, doctors are trained to believe that nutrition and weight loss are simply not part of the problems that doctors should deal with or care about. Medical students model their own self-image as a doctor on their mentors they meet in medical school. And those doctors and those researchers simply didn’t care about nutrition or weight loss.
This contrasts starkly with the medical knowledge that they learn. Everybody, and certainly every medical student, knows that obesity plays a dominant role in metabolic diseases like type 2 diabetes and the metabolic syndrome. In turn, these metabolic diseases raise the risk of heart disease, stroke, cancer, kidney disease, blindness, amputations etc. Doctors understood fully the importance of weight gain for disease. They just didn’t care to know any more about how to lose weight or what we should or should not eat.
Here’s what a normal person would think.
- Weight gain leads to metabolic disease and then heart attacks (or type 2 diabetes, or joint pain or a million other ailments related to weight)
- What can I do to prevent or reverse weight gain (the root cause)?
Here’s how a doctor is trained to think:
- Weight gain leads to metabolic disease and then heart attacks
- What drugs or surgery should I give to patients after they have their heart attack?
You would be entirely correct here in thinking “what the heck?”
Everybody knew full well how obesity and metabolic disease are destroying our nation’s health, medical schools were not teaching medical students how to treat this. Instead, they gave the unmistakable message that weight loss was not something doctors should care about, learn about, or try to achieve with their patients. Doctors often tell patients to lose weight. What they don’t often tell patients, however, is how to lose weight.
Cut the calories
The entire medical school curriculum about weight loss was about as insightful as your latest issue of Cosmopolitan magazine. Eat less. Move more. Cut about 500 calories per day and you will lose about a pound of fat per week.
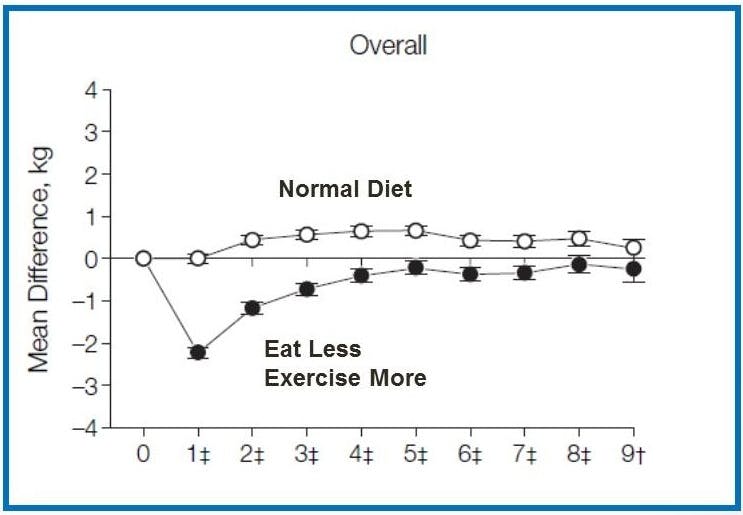
If this were a new drug, for say, lung cancer, then doctors would immediately want to know – does it work? For weight loss, we learned about this calorie-cutting method, but nobody seems to ask out loud – does it work? We already knew that it did not. After all, everybody had already tried this weight loss method for the last 50 years and it worked for nobody.
There were controlled trials of the calorie restriction method for weight loss. Almost every single study failed. There were thousands of real-world patients who tried it. The success rate was about 1%. Doctors were trained to give weight loss advice that had an expected failure rate of 99%. What boggles the mind is why doctors don’t stop and think why they are giving advice that is expected to fail 99% of the time. The most unfair part is that when patients do return, unable to lose weight, the doctor then blames them for their failure. It’s so much easier to blame the patient than the find fault with the standard medical advice of cutting calories.


Medical students are subjected to an enormous unconscious bias. They see that all the doctors they know, all the doctors that teach them, all the doctors in the hospital don’t care really about nutrition or giving weight loss advice. Therefore, they understand that this is not something that doctors ‘do’. We give medications. We do surgery. We don’t ‘do’ weight loss. Even if it is the root cause of most of the disease we see today.



Talk to your doctor about weight loss? Would you ask your plumber to remove your wisdom teeth? Would you ask your barista to check your vision? It doesn’t have to be this way, of course. The obvious thing to do is include more nutrition into the curriculum of medical school or residency training. It would also help if doctors learned a bit more of the physiology behind weight loss and weight gain. About the hormonal regulators of weight, and how to influence them using diet. In my experience, weight gain is a hormonal, not a caloric, imbalance.
Also published on idmprogram.com.
Dr. Fung’s top posts
Type 2 diabetes
Weight loss
Keto
Intermittent fasting
More with Dr. Fung
Dr. Fung has his own blog at idmprogram.com. He is also active on Twitter.
Dr. Fung’s books The Obesity Code, The Complete Guide to Fasting and The Diabetes Code are available on Amazon.




















































































