The scale and its other liar acolytes

We’ve been conditioned to step on a scale to check whether we’re gaining or losing weight. Some do it every day, others every now and then. Some have actually buried their scale deep in a closet, never to be seen again, while others have tossed it the garbage bin, or may even have set it on fire.
In our low-carb clinic, we weigh patients at every visit. It is, indeed, one of the markers of progress. It’s the one everyone cares about, but it’s the least reliable one. It lies all the time about the progress being made. It can be discouraging, especially for those who have been eating clean keto for weeks.
What we tell patients
Here’s what we tell patients:
- Your body contains a lot of water, and it tries to keep it stable, within 2 litres. One litre of water is around 2 pounds or 1 kg. If you’ve just drank a lot of water, you will weigh more. If you just exercised, you might weigh less. It’s just water.
- Patients usually weigh themselves at home, in their birthday suit. We prefer not to do that in the clinic. Clothes can easily add around 2 pounds (1 kg).
- Different scales give different readings. There can be a significant difference between the scale used at home and the scale in my office. I learnt that the hard way when my 5-pound (2 kg) newborn baby girl was “losing too much weight” on one scale in a pharmacy, and “gaining just right” on the scale at the clinic. One result nearly sent us back to the hospital in a panic (you know, first time parents panic easily), while the other one made us sigh in relief. Using the same scale all the time helps.
- Muscles weigh more than fat but use less space. My patients get a complete evaluation with Marc Ciminelli, our kinesiologist, about halfway through their 6-month-program. At that point, usually, they feel so much better, they are really eager to get moving. As they start exercising according to their capabilities, we often see the weigh loss slow down on the scale. Some patients get really discouraged because of that. They are used to measuring progress with the scale. Nurse Sylvie constantly reminds them that centimeters off the waist are a much better marker of progress, and a much better marker of metabolic health.
- The days after an intense weight-training program, you may also weigh more, as your muscles are sore and a bit swollen.
- Exercising and eating healthy can help increase bone density. If your bones get denser, they get heavier.
- Carbs can cause water retention. If you’ve indulged in something high carb, you will likely retain water. Insulin causes water retention. One slice of bread did not make you gain 4 pounds (2 kg) of fat overnight.
- Constipation can cause an excess of 1 to 4 pounds (0.5-2 kg).
- Hormonal changes can cause temporary water retention.
- Etc.
So, the scale is a big liar when it comes to telling the whole story of progression. It’s one of the biggest liars in my opinion. But there are others. And those can be deceiving not only for the patients, but for the doctors as well.
Centimeters off the waist
In our clinic, we also measure cm or inches lost around the waist. To be accurate, we measure at the belly button (not the actual waist), trying to maintain a horizontal line with the tape measurer, so that it’s easily reproducible from one visit to the next. We know that central obesity (think “beer belly”) is a strong marker of metabolic disease, like insulin resistance, fatty liver, chronic inflammation, etc. Waist circumference is one of the recognized official criteria of metabolic syndrome.
Losing centimeters off the waist is a much better marker of health improvement than is the scale. And those two don’t necessarily go hand in hand. It is very frequent to see a loss of numerous centimeters while the scale doesn’t move a notch.
Patients are disappointed when the scale doesn’t budge. Sylvie reminds them that centimeters are a greater victory. They half-smile. Their minds still mainly care about the number on the scale. Switching that mindset is a constant work in progress.
But centimeters can lie too.
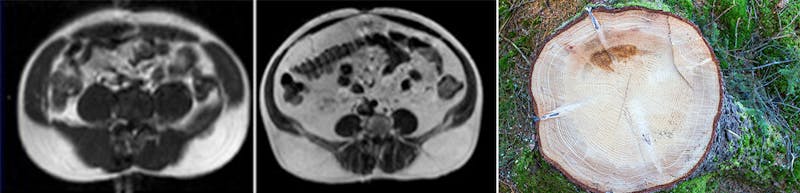
These are scans of two patients with the same waist circumference. To understand what you are looking at, imagine looking at all the circles inside a sawn tree.
On the left, you see a fair amount of muscles. It’s the black oval shapes you see right underneath the white outer layer of fat.
On the right, you can see a very thin layer of muscles under the fat. You can also see a LOT of white fat inside the abdominal cavity. It’s all around and inside the organs. We call these people TOFI, which means thin on the outside and fat on the inside. A TOFI can look normal or healthy, but that is deceiving.
Below are eight examples of men with the same waist circumference.
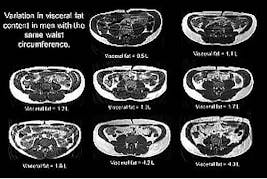


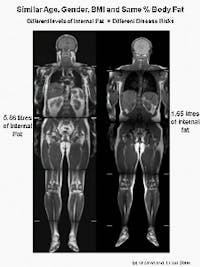


So, losing centimeters is wonderful as a marker of improved metabolic health. But the actual number of centimeters can not always be trusted. Don’t assume a person is healthy or doesn’t have type 2 diabetes just because he or she has a waist circumference that doesn’t meet the metabolic syndrome criteria.
Lipid panels
At our low-carb clinic, we do extensive blood work with every patient at the beginning of the program, at 3 months and at 6 months. Amongst other things, we check and follow lipid markers. Not just LDLs, of course. As Dr. Ken Sikaris would say (check out his wonderful videos about lipids on YouTube) “If you only care about LDLs, you’re 30 years behind”. To fully grasp how right he is about this, check out The Cholesterol Code.
For all kinds of reasons, when people embark on a low carb or keto journey, and especially if they have a fatty liver and/or a lot of weight to lose, the first few lipid panels can give all kinds of scenarios, encouraging or worrisome. Sometimes it’s just a lab fluke. You or your doctor must not interpret this as a proof that low carb isn’t good or isn’t working for you. For the vast majority of patients, lipid markers will normalise eventually, and show significant improvements compared to baseline. It may need time.
HbA1c or A1c
Here’s another liar: glycated hemoglobin. It is a form of hemoglobin (red blood cells) that is measured basically to estimate someone’s average sugar level over the last 3 months. It’s particularly useful with patients with diabetes. Patients who eat less carbs, and therefore less sugar, expect their HbA1c to go down. But it can also be a liar.
If you have diabetes and on any number of sugar-lowering drugs, including insulin, your sugar levels are indeed expected to go down as you start eating low carb. They will go down to near normal, at which point I will reduce or eliminate one of your drugs. Your sugar levels will rise back up a bit (below 12 at all times is my goal). As you keep eating low carb, they will go down again. I will reduce or eliminate another drug. The sugar levels will temporarily rise a little again, but will go down eventually, and so on and so forth. The goal being to eliminate all diabetes medication if possible (as well as most anti-hypertensives).
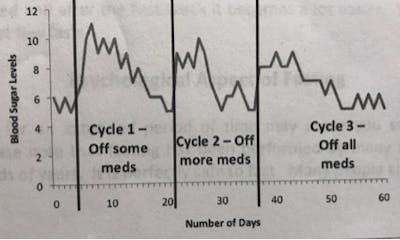


So, when HbA1c is measured in the middle of this waltz, it is possible that it shows a higher value than the previous one. Does it mean it’s not working? Certainly not. If the latest value was achieved with, say, 2 or 3 drugs discontinued, then it’s definitely working.
So, for any patient eating low carb, and for any doctor following patients on a low-carb journey, I think it is essential to measure progress with more than one marker, and to give the whole process of disease reversal enough time to see the emergence of a trend. Allow for bumps on the road, inexplicable ups and downs, markers that temporarily go in the wrong direction. Focus on feeling well, not so much on the scale or on its other lying friends.
Remember that no one got diabetes or overweight overnight. It took time to get sick, it will take some time for your body to get healthy again. Just keep on low carbing it. And consider putting the scale away for a while.
More
Earlier with Dr. Bourdua-Roy
All earlier posts by Dr. Bourdua-Roy



































































