Type 2 diabetes – What happened and how we can fix it
Although diabetes isn’t a brand new disease, the world wide epidemic of the disease is relatively new. How did we get here? And more importantly, can understanding how we got here help us correct the course? We think the answer is yes. And that simple answer could improve millions of lives.
This guide explains the background of how our food choices may have led us down this path and shows the beginnings of a way out. For more details about diabetes, please see out detailed guides about type 1 diabetes, type 2 diabetes, symptoms of diabetes, the best foods to eat to reverse diabetes.
With a properly planned low-carb diet, you may be able to normalize your blood sugar naturally — with less or even no medication, and without calorie counting or hunger. Many people have already done so, and studies have confirmed it.1 So, keep reading to see if this could work for you!The main potential danger regards medications, where doses may need to be adapted. In particular, insulin doses may need to be lowered to avoid low blood sugar, and SGLT2 inhibitors may need to be de-prescribed. Learn more
Discuss any changes in medication and relevant lifestyle changes with your doctor. Full disclaimer
A disastrous epidemic
What’s wrong? Why are more and more people developing type 2 diabetes?
In the past, before our modern Western diet, type 2 diabetes was extremely rare.2 The disease is now becoming more common around the world:

Statistics: WHO and IDF
The number of people with diabetes is increasing rapidly and is heading towards 500 million, with one estimate suggesting we are already there.3This is a worldwide epidemic. Will someone in your family be affected next? Or could it even be you?
Many people diagnosed with the most common form of diabetes (type 2) never regain their previous health. Instead, the “natural course” is that they are expected to become a little sicker every year, needing more and more drugs.4 And at some point serious complications may emerge: Blindness. Dialysis due to faulty kidneys. Dementia. Amputations. Death.5
Fortunately, there’s something you can do about it. By understanding the factors that have led to the explosion of this disease you can help yourself or others with diabetes regain health.
Reversed dietary guidelines
Dietary advice in recent decades has looked similar throughout the Western world. While more people have gotten type 2 diabetes and have required higher doses of medications, they’ve been advised to eat foods that commonly raise blood sugar.
Here’s a good example, the Swedish Plate Model for people with type 2 diabetes, which is similar to the My Plate in the U.S.:




Which sections of the plate can raise blood sugar the most? Those that contain carbohydrates (sugar and starch).
Bread and potatoes consist of starch, milk contains lactose (milk sugar) and fruit contains fructose and glucose (plain sugar):
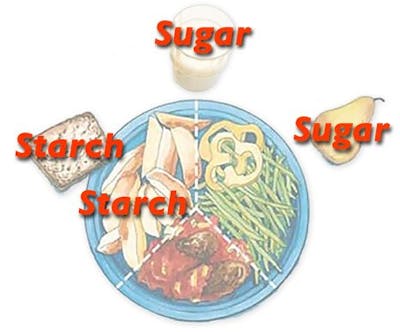



Since the food pictured above can potentially raise blood sugar, eating this may not improve the health of people with diabetes as well as diets restricting those foods.6
Studies examining similar carbohydrate-rich dietary advice suggest there may be an increased risk of developing diabetes and potentially worsening blood sugar levels long term compared to a lower-carbohydrate diet.7 Perhaps that’s why this advice hasn’t been shown to improve health in other important ways such as decreasing heart disease risk.8
Fear of natural fat is one potential driving force behind the continued high-carb recommendations. Avoiding fat frequently means increasing carbohydrates in order to provide energy and satiety. But in recent years the theory about fat being dangerous has been scientifically questioned.
Is there an alternative that will produce better health and weight with foods that don’t raise blood sugar?
Old wisdom
Is the low-carbohydrate diet for people with type 2 diabetes a new invention? It definitely isn’t. There’s long-time experience of the positive effects, which Harvard researcher Dr. David Ludwig and colleagues reviewed in their 2021 publication.9
In the past, before there was insulin or medication to lower blood sugar, diet was the only strategy for managing diabetes.10
Here are pictures from a cookbook for people with diabetes from 1917. You can read the entire book for free online. Below is an image of pages 12-13, where there’s a summary of what they should and should not eat.
Let’s start with what people with type 2 diabetes were advised not to eat a hundred years ago.
Strictly forbidden foods
The title of the page is “Foods Strictly Forbidden.” It starts with sugars and “All Farinaceous Foods and Starches” — in other words, foods made of flour and other starches. Examples follow:
- Bread
- Cookies
- Rice
- Pasta
- Sweet drinks
Some of these strictly forbidden foods are now part of the recommended diabetes diet from many medical organizations. Although correlation does not prove causation, it is interesting that the progressively higher carb intake recommendations occurred at the same time as rising diagnoses of type 2 diabetes.11
Especially valuable foods
Here’s the list of recommended nutrient-dense diabetes foods: Butter, olive oil, cheese, meat, fish, eggs…
This sounds familiar. If we just add generous amounts of vegetables, this will be a nearly complete list of low-carb foods. This is the advice most low-carb physicians give to their patients with type 2 diabetes. They routinely see improved blood sugar, weight loss, and reduced need for medications.12
So why don’t more people get the old advice?
New science
The carbohydrate-rich dietary advice given to people with type 2 diabetes in recent years is likely based on the misguided fear of naturally fatty foods.13 But, when it comes to type 2 diabetes, there are no quality studies showing that a carb-rich diet is more beneficial than a low-carb diet.
It’s actually the opposite. Many studies show that LCHF and keto diets are as good as, or in some cases even better for blood sugar and weight than today’s low-fat advice.14Even the American Diabetes Association now acknowledges that a low-carbohydrate diet is the most effective diet for normalizing blood sugar in those with diabetes.
And this makes sense. Now that we know how we got here, we can start to see how to fix it. We are pleased to see organizations such as the ADA recognizing the importance of reducing carbohydrates.
Read more in our guide that will show you the best foods to eat to reverse diabetes.
A tale of two meals
How much is your blood sugar affected by the food you eat? A lot. Here’s an example of how significant the difference can be:




The picture to the left is a typical LCHF meal: steak fried in butter, vegetables fried in butter, and a homemade béarnaise sauce (melted butter and egg yolk). Lots of fat, an ample amount of protein, but almost no carbohydrates.
In the picture to the right you can see the lunch that was served at the 11th International Congress on Obesity in Stockholm 2010. This is a major international conference for obesity doctors and scientists. The food contains almost exclusively energy from sugar and starches, things that are broken down to simple sugars in the digestive tract.
Let’s see what impacts the two meals had on blood sugar:15
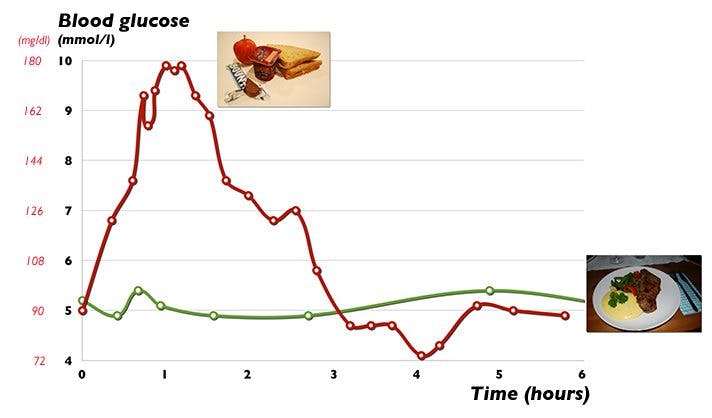



A blood glucose level between 70-100 mg/dl (4-6 mmol/l) is typical while fasting. It can then rise after a meal, depending how much carbohydrate you eat.
As you can see, the blood sugar did not change after the LCHF meal (green line). Not really surprising. If you don’t eat many carbohydrates, not a lot of glucose will reach the bloodstream, and consequently the blood glucose level will remain stable.
By contrast, blood sugar after the lunch at the obesity conference shot through the roof (red line), all the way up to 180 mg/dl (9.9 mmol/l), in just an hour.
Want to do a similar test yourself? Order a simple blood glucose meter and test strips here.
Become your own evidence
A growing tide of people are reacting to the latest evidence, understanding how it differs from some outdated guidelines, and taking command of their own health.
Do you want to learn the truth for yourself? Luckily, there’s a very simple way to find out what effect a low-carbohydrate diet will have on you.
Try it yourself for a few weeks and monitor the effect. Simply test your blood sugar before you eat, then eat a “regular” carb meal, and then recheck your blood 1 and 2 hours after you eat. If it is still elevated at 2 hours, keep checking until it returns to baseline. Then do the same for a low-carb meal. Even better, stick with low carb for a couple of weeks and see how it continues to improve. You can get started with our 2-week keto challenge.
Here are some success stories from people who have seen transformative health benefits, including:16
- Improved blood sugar levels, starting from the first meal
- Increased satiety and weight loss, often noticeable already within a week
- Reduced sugar cravings
Take command of your own health and test it for yourself:
Start the journey
This is a 45-minute video of Dr. Andreas Eenfeldt’s presentation from the Low Carb USA conference in 2017, explaining much of the case for low carb for people with type 2 diabetes.
How to reverse type 2 diabetes
Is it possible to reverse type 2 diabetes? Doctor Jay Wortman, M.D., knows more about this than most people. He developed type 2 diabetes himself, but after a simple dietary change, he’s reversed his diabetes with no need for medications.
Jay Wortman also did a spectacular study on native Canadians. When they went back to eating traditional foods their Western diseases went away.
Above is a 25-minute interview I did with Dr. Wortman.
Links
Dr. Wortman’s website and blog
Books:
More from the Diet Doctor
Selected blog posts on diabetes from the last few years:
Type 2 diabetes – What happened and how we can fix it - the evidence
This guide is written by Dr. Andreas Eenfeldt, MD and was last updated on June 19, 2025. It was medically reviewed by Dr. Bret Scher, MD on February 9, 2022.
The guide contains scientific references. You can find these in the notes throughout the text, and click the links to read the peer-reviewed scientific papers. When appropriate we include a grading of the strength of the evidence, with a link to our policy on this. Our evidence-based guides are updated at least once per year to reflect and reference the latest science on the topic.
All our evidence-based health guides are written or reviewed by medical doctors who are experts on the topic. To stay unbiased we show no ads, sell no physical products, and take no money from the industry. We're fully funded by the people, via an optional membership. Most information at Diet Doctor is free forever.
Read more about our policies and work with evidence-based guides, nutritional controversies, our editorial team, and our medical review board.
Should you find any inaccuracy in this guide, please email andreas@dietdoctor.com.
The European Journal of Clinical Nutrition 2017: The interpretation and effect of a low-carbohydrate diet in the management of type 2 diabetes: a systematic review and meta-analysis of randomised controlled trials [strong evidence]
Frontiers in Endocrinology 2019: Long-term effects of a novel continuous remote care intervention including nutritional ketosis for the management of type 2 diabetes: a 2-year non-randomized clinical trial [non-randomized trial; weak evidence]
Diabetes, Obesity & Metabolism 2019: Low versus high carbohydrate diet in type 1 diabetes: A 12-week randomized open-label crossover study [moderate evidence]
Asia Pacific Journal of Clinical Nutrition 2016: A randomised trial of the feasibility of a low carbohydrate diet vs standard carbohydrate counting in adults with type 1 diabetes taking body weight into account [moderate evidence]
↩Although diabetes was first recognized thousands of years ago, up until recently most cases were due to insulin deficiency, a hallmark of type 1 diabetes:
The New England Journal of Medicine 2012: The past 200 years in diabetes [overview article; ungraded] ↩
Diabetes research and Clinical Practice 2019: Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: Results from the International Diabetes Federation Diabetes Atlas, 9 th edition [review of observational studies, weak evidence]
Diabetes 2018: Global prevalence of type 2 diabetes over the next ten years (2018-2028) [review of observational studies; weak evidence]
Medicine 2014: Epidemiology of diabetes [review of observational studies; weak evidence] ↩
Diabetes Care 2013: Clinical inertia in people with type 2 diabetes [observational study, weak evidence]
Population Health Management 2017: Diabetes 2030: Insights from yesterday, today, and future trends [overview article; ungraded] ↩
Journal of Diabetes Research 2018: Complications of diabetes 2017 [observational study, weak evidence] ↩
The following RCT demonstrated a low-carb diet better controls blood sugar compared to a low-glycemic index diet.
Nutrition and Metabolism 2008: The effect of a low-carbohydrate, ketogenic diet versus a low-glycemic index diet on glycemic control in type 2 diabetes mellitus. [randomized trial; moderate evidence]
instead of improving, eating higher carb diets may cause blood sugar to gradually increase over time, requiring more medication to control it. More medication can lead to greater obesity since weight gain is a well-known side effect of insulin and some oral diabetes medications:
Journal of Obesity 2011: Weight considerations in pharmacotherapy for type 2 diabetes [overview article; ungraded] ↩
Compared to a higher-fat Mediterranean diet, conventional low-fat advice resulted in more people developing diabetes:
Diabetes Care 2011: Reduction in the incidence of type 2 diabetes with the Mediterranean diet [moderate evidence] ↩
NEJM 2013: Cardiovascular effects of intensive lifestyle intervention in type 2 diabetes [randomized trial; moderate evidence]
National Institute of Health 2012: Weight loss does not lower heart disease risk from type 2 diabetes[moderate evidence]
↩Journal of Clinical Investigations 2021: Carbohydrate restriction for diabetes: rediscovering centuries-old wisdom[overview article; ungraded] ↩
At the time, type 1 and type 2 diabetes hadn’t yet been identified as different diseases, and some doctors prescribed very-low-carb diets for all patients with diabetes:
Perspectives in Biology and Medicine 2006: Dietary treatment of diabetes mellitus in the pre-insulin era (1914-1922) [overview article; ungraded] ↩
The timing and correlation was described in the following review article:
Journal of the History of Medicine and Allied Sciences 2008: How the ideology of low fat conquered America [overview article; ungraded]
It has also been well documented in popular books such as The Big Fat Surprise by journalist Nina Teicholz and Good calories, Bad Calories by journalist Gary Taubes.
↩This is based on clinical experience of low-carb practitioners and was unanimously agreed upon by our low-carb expert review panel. You can learn more about our panel here [weak evidence].
It is also supported by randomized and nonrandomized clinical trials.
Nutrition and Diabetes 2017: Twelve-month outcomes of a randomized trial of a moderate-carbohydrate versus very low-carbohydrate diet in overweight adults with type 2 diabetes mellitus or prediabetes [randomized trial; moderate evidence]
Frontiers in Endocrinology 2019: Long-term effects of a novel continuous remote care intervention including nutritional ketosis for the management of type 2 diabetes: A 2-year non-randomized clinical trial [weak evidence]
↩Although there’s still disagreements among some experts, several large systematic reviews of clinical trials have found no evidence that saturated fat increases risk of heart disease, early death, or other health issues:
Nutrition Journal 2017: The effect of replacing saturated fat with mostly n-6 polyunsaturated fat on coronary heart disease; a meta-analysis of randomized controlled trials [strong evidence]
Read more in our guide on saturated fat.
↩Nutrition Reviews 2022: Effect of a very low-carbohydrate ketogenic diet vs recommended diets in patients with type 2 diabetes: a meta-analysis [strong evidence]
International Journal of Endocrinology 2021: Comparing the efficacy and safety of low-carbohydrate diets with low-fat diets for type 2 diabetes mellitus patients: a systematic review and meta-analysis of randomized clinical trials [strong evidence]
The American Journal of Clinical Nutrition 2018: Effects of low-carbohydrate- compared with low-fat-diet interventions on metabolic control in people with type 2 diabetes: a systematic review including GRADE assessments [strong evidence]
The British Journal of Nutrition 2016: Effects of low-carbohydrate diets v. low-fat diets on body weight and cardiovascular risk factors: a meta-analysis of randomised controlled trials [strong evidence]
PLoS One 2015: Dietary intervention for overweight and obese adults: Comparison of low-carbohydrate and low-fat diets. A meta-analysis [strong evidence] ↩




