Signs and symptoms of diabetes (type 1 and 2)
Over the past 40 years the number of people with diabetes worldwide has quadrupled and currently stands at more than 400 million, according to the World Health Organization (WHO). What’s more, many are unaware they have diabetes or its precursor, prediabetes.1
Could you have diabetes? It’s a disease with many possible symptoms, although it is often clinically silent early on in its course. When symptoms are present, some are subtle while others are hard to ignore. Read on to learn about the most common symptoms of diabetes and what you can do if you have them.
1. What is diabetes?
Diabetes is a medical condition that causes high blood sugar due to a lack of insulin (a hormone that controls blood sugar) or an inability to use it effectively – or both. Although it can take several forms, type 1 and type 2 are by far the most common.
- In type 1 diabetes, the body’s immune system mistakenly destroys cells in the pancreas that make insulin.2 Because of this, people with type 1 diabetes can no longer make insulin on their own and must inject it every day — not only to control blood sugar but also to survive.
- In type 2 diabetes, there are defects in both the production of insulin by the pancreas (insulin deficiency) and the use of insulin by the body (insulin resistance). When damage to the pancreas’ insulin-producing cells progresses to the point where the pancreas can no longer spontaneously release enough insulin to overcome the body’s resistance to it, blood sugar levels rise.3
A related and very important condition is prediabetes, in which blood sugar is higher than normal but not high enough to be classified as diabetes. Additionally, insulin levels are usually elevated both before and after eating.4
Over time, prediabetes may progress to type 2 diabetes; however, it carries some of the same health risks of diabetes even if blood sugar remains in the prediabetes range.5
Although people with prediabetes usually don’t have symptoms that one might have with very high blood sugar, they may have some of the more subtle ones.
2. Symptoms of diabetes
Here are the most common diabetes symptoms:
- Thirst and urination
- Fatigue
- Hunger
- Weight loss
- Delayed healing
- Blurred vision
- Numbness
- Dark patches
- Skin rashes
- Yeast and urinary tract infections
- Erectile dysfunction
You may have one, two, or several symptoms — or you may have none. An absence of symptoms doesn’t mean an absence of diabetes.6
However, being aware of common symptoms may lead to diagnosis much earlier, which may help prevent long-term complications.
Increased thirst and urination
 Have you been feeling very thirsty or running to the bathroom more often lately? Frequent urination coupled with a near-constant sensation of thirst are well-known symptoms of diabetes.7
Have you been feeling very thirsty or running to the bathroom more often lately? Frequent urination coupled with a near-constant sensation of thirst are well-known symptoms of diabetes.7
When blood sugar is too high, water is pulled from your bloodstream and organs to help your kidneys flush out the excess glucose.
The sugary urine smells sweet – and even tastes sweet. In fact, although it’s rather unsettling to think about, tasting patients’ urine helped doctors identify diabetes before blood tests and glucose meters were available.
Because so much water is leaving your body, the brain triggers your thirst mechanism, prompting you to drink enough to replace what’s being lost.
Excessive thirst and urination is more common in type 1 diabetes when blood sugar levels are very high but may also occur in type 2 diabetes.8 In a study of over 1,100 people recently diagnosed with type 2 diabetes, more than half reported increased urination, and nearly two-thirds reported being abnormally thirsty.9
Severe fatigue
Although there are many conditions that can make you feel tired, diabetes is a very common one. In undiagnosed diabetes, fatigue is tough to ignore; you may feel so tired that you can barely keep going during the day, despite getting plenty of sleep.
Why does diabetes make you feel so tired? One theory is because glucose — one of your body’s major fuel sources — is accumulating in your bloodstream rather than getting into your cells.10
Insulin allows glucose to enter your cells. When your pancreas doesn’t produce insulin or your cells are resistant to its effects, glucose remains in the blood. As a result, you may feel tired and weak because your cells are deprived of the fuel they need.11
In studies, many people with newly diagnosed diabetes report fatigue as one of their main symptoms.12
Feeling hungrier than usual
It’s normal for your appetite to vary from day to day based on activity, sleep, mood, and dozens of other factors. However, if you’ve recently been much hungrier than usual, diabetes could be the reason.
Along with frequent urination (polyuria) and thirst (polydipsia), severe hunger (polyphagia) is one of the “Three P’s” considered to be classic symptoms of diabetes.13
Unfortunately, eating more food usually doesn’t satisfy this hunger. What’s more, reaching for carbohydrate-rich foods (including fruit, legumes, and whole grains) can cause blood sugar to increase even more.14
This is because starchy carbohydrates like cereals, potatoes or bread are made up of lots of glucose molecules joined together. The process of digestion breaks these starches back down into glucose, which raises blood sugar once it’s absorbed into the bloodstream.15
Although it can also happen in type 2 diabetes, feeling noticeably more hungry is especially common in type 1 diabetes.16
Unexplained weight loss




Everyone experiences small weight fluctuations from day to day, but if you’ve lost 10 pounds (4.5 kilos) or more without trying, diabetes may be the cause.
In addition to allowing glucose to enter your cells and preventing your liver from releasing glucose, insulin helps prevent muscle and fat breakdown.
If you have type 1 diabetes, your pancreas makes little to no insulin. Therefore, your body begins to break down fat and muscle, leading to weight loss.
Although unexplained weight loss is much more common in people with type 1 diabetes — including children and lean adults who can’t afford to lose weight — it can also happen in those with type 2 diabetes.
In one study, slightly more than one-third of people newly diagnosed with type 2 diabetes reported that they had recently lost weight without trying.17 Furthermore, one study found that some populations with type 2 diabetes may experience unintentional weight loss more often than others.18
Delayed healing of injuries
Have you noticed that cuts, scrapes, or other injuries have been taking longer to heal than usual? This may be a warning sign of diabetes. Elevated blood sugar has been shown to interfere with proper wound healing following surgery or injury.19
Why would having high blood sugar prolong the time it takes your skin to heal? Research suggests that elevated blood sugar drives inflammation and impairs the immune system’s ability to repair wounds effectively.20 In addition, decreased blood flow from peripheral artery disease can further impair wound healing.21 So if blood sugar levels are high, minor injuries might take weeks or months to heal rather than days.
Blurred vision




Elevated blood sugar causes the lens of the eye to swell, which can change its shape. When this occurs, the lens can no longer focus light properly, causing distance vision to become blurry.22
High blood sugars can also impair the function of one or more of the nerves that control eye muscle movements, leading to blurry vision.23
Once blood sugars return to healthier levels, the lens goes back to its usual shape, the nerves start working better, and vision becomes normal again.
In one study, about one quarter of people with newly diagnosed diabetes reported that their vision had become blurry.24
Numbness and tingling in feet or toes
It’s normal to have that familiar yet uncomfortable “pins and needles” sensation after sitting too long or putting pressure on one part of the body. However, if it occurs in your feet or toes for no apparent reason, diabetes or prediabetes could be responsible.
Elevated blood sugar can damage the nerves leading to your feet, resulting in numbness and tingling. The medical term for this condition is diabetic peripheral neuropathy.25
Importantly, blood sugar may not need to be very high for this damage to occur.
In one study, 49% of people with prediabetes and 50% of those with newly diagnosed diabetes were found to have peripheral neuropathy.26Other studies have shown lower – but still significant – incidences of neuropathy in people with prediabetes and diabetes.27
Dark patches of skin
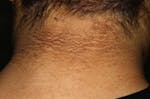



The medical term for these patches is acanthosis nigricans. It may be caused by several conditions but is often linked to elevated insulin levels and insulin resistance.28 It has also been linked to type 2 diabetes, especially in those who are overweight or obese.
In one study of people newly diagnosed with type 2 diabetes, 54% of those who were obese had acanthosis nigricans.29
Skin lesions or rashes
Rashes, lesions, and other skin problems may be an early warning sign of diabetes.
Several skin conditions — including eruptive xanthomatosis, necrobiosis lipoidica, and diabetic dermopathy — are characterized by itchy rashes or painful blisters that appear when blood sugar is too high.
Although the precise mechanism behind these and other skin disorders in people with diabetes isn’t clear, elevated blood sugar may lead to inflammation and interfere with the ability to grow healthy new skin cells to replace old ones.30
One large review of existing studies found that over 50% of people with diabetes worldwide had some type of diabetes-related skin disorder.31
Yeast and urinary tract infections (women)
Have you been experiencing yeast infections or urinary tract infections (UTIs) more often lately? Frequent infections may be an early warning sign of diabetes, with yeast infections and UTIs among the most common.
High blood sugar can fuel the growth of both Candida (the fungus responsible for vaginal yeast infections) and several types of bacteria that can cause UTIs. In addition, high blood sugar levels may depress immune function, making your body more susceptible to these infections.32
Erectile dysfunction (men)
In men, one of the first signs of diabetes may be difficulty with sexual function. High blood sugar can affect the nerves and blood vessels that supply the reproductive organs, resulting in erectile dysfunction.
Studies suggest that men who have diabetes may be three to five times more likely than other men to have erectile dysfunction.33
3. How to find out if you have diabetes
If you have one or more of the symptoms above and suspect you may have diabetes, it’s important to make an appointment with your doctor or primary care provider. They will examine you and order lab tests to confirm whether you have type 1 diabetes, type 2 diabetes or prediabetes, and to rule out other causes of your symptoms.
You can also test your blood sugar at home to see if it is elevated. Regardless of the results, be sure to follow up with your healthcare provider if you have any symptoms of diabetes.
Importantly, in many cases, you may have no obvious symptoms of prediabetes or early-stage type 2 diabetes.
4. What can you do if you have diabetes or prediabetes?
If you’ve been diagnosed with diabetes or prediabetes, you’re likely to be upset and concerned.
Although this is completely understandable, take heart. In addition to following up with your doctor on a regular basis, there are steps you can take right now to get your blood sugar under control — and make sure it stays there.
In fact, in many cases, type 2 diabetes and prediabetes can be reversed or put into remission with a low-carb diet alone.34 Check out our guide below.35
And although type 1 diabetes can’t be reversed, low-carb eating can help control blood sugar.36 See our guide below.
Finally, please don’t ignore the symptoms of diabetes, no matter how subtle they seem. It’s never too early to see your doctor and get checked out — or to start following a low-carb diet to achieve healthy blood sugar levels.
Furthermore, even if your blood sugar is normal now, limiting sugary and starchy foods may help to keep it that way. This doesn’t mean going on a diet – just eating better. Take a look at our guide below on six steps you can take to eat fewer carbs.
Videos about diabetes
Signs and symptoms of diabetes (type 1 and 2) - the evidence
This guide is written by Franziska Spritzler, RD, Dr. David Unwin and was last updated on June 19, 2025. It was medically reviewed by Dr. David Unwin on July 21, 2021 and Dr. Bret Scher, MD on July 28, 2022.
The guide contains scientific references. You can find these in the notes throughout the text, and click the links to read the peer-reviewed scientific papers. When appropriate we include a grading of the strength of the evidence, with a link to our policy on this. Our evidence-based guides are updated at least once per year to reflect and reference the latest science on the topic.
All our evidence-based health guides are written or reviewed by medical doctors who are experts on the topic. To stay unbiased we show no ads, sell no physical products, and take no money from the industry. We're fully funded by the people, via an optional membership. Most information at Diet Doctor is free forever.
Read more about our policies and work with evidence-based guides, nutritional controversies, our editorial team, and our medical review board.
Should you find any inaccuracy in this guide, please email andreas@dietdoctor.com.
In the US alone, nearly one quarter of all people with diabetes and more than 80% of those with prediabetes don’t know they have the disease:
Centers for Disease Control and Prevention: National Diabetes Statistics Report 2017 [report; ungraded]
↩Immunity 2010: Etiology of type 1 diabetes [overview article; ungraded] ↩
Journal of Clinical Endocrinology and Metabolism 2001: Clinical review 135: The importance of beta-cell failure in the development and progression of type 2 diabetes. [overview article; ungraded]
Frontiers in Endocrinology 2013: Beta cell dysfunction and insulin resistance. [overview article; ungraded]
↩The high insulin levels reflect the pancreas trying to make enough insulin to overcome the body’s resistance to it; this just barely keeps the blood sugar normal or slightly above normal, for a time. Once the pancreas can no longer keep up with this demand, insulin levels fall, blood sugar rises, and prediabetes becomes diabetes. ↩
Minerva Medica 2019: Treating prediabetes: why and how should we do it? [overview article; ungraded]
Among people with prediabetes, high blood sugar levels after eating have been linked to greater risk of heart disease:
Diabetes Care 1999: Impaired glucose tolerance is a risk factor for cardiovascular disease, but not impaired fasting glucose: the Funagata diabetes study [observational cohort study with RR > 2.0; weak evidence]
↩In one study, more than 40% of people newly diagnosed with type 1 or type 2 diabetes stated they hadn’t noticed any symptoms of the disease prior to diagnosis:
Diabetes Care 2007: Symptoms of diabetes and their association with the risk and presence of diabetes [observational study; very weak evidence] ↩
Diabetes care 2007: Symptoms of diabetes and their association with the risk and presence of diabetes: findings from the Study to Help Improve Early evaluation and management of risk factors Leading to Diabetes (SHIELD) [anecdotal report; very weak evidence] ↩
Diabetes Care 2007: Symptoms of diabetes and their association with the risk and presence of diabetes [observational study; very weak evidence] ↩
Diabetologia 2005: Symptoms, signs and complications in newly diagnosed type 2 diabetic patients, and their relationship to glycaemia, blood pressure and weight [observational study; very weak evidence] ↩
This is based on theory. There is no scientific evidence proving why someone with diabetes feels fatigued. ↩
Advances in Biochemical Research 2017: Biochemico-physiological mechanisms underlying signs and symptoms associated with diabetes mellitus [overview article; ungraded] ↩
Diabetes Care 2007: Symptoms of diabetes and their association with the risk and presence of diabetes [observational study; very weak evidence]
Diabetologia 2005: Symptoms, signs and complications in newly diagnosed type 2 diabetic patients, and their relationship to glycaemia, blood pressure and weight [observational study; very weak evidence] ↩
Point of care 2017: Type 1 diabetes – A clinical perspective [overview article; ungraded] ↩
Research has confirmed that high-carbohydrate foods raise blood sugar levels in people with diabetes as well as those without diabetes:
Diabetes Care 2004: Dietary carbohydrate (amount and type) in the prevention and management of diabetes [overview article; ungraded]
The Journal of Nutrition 1996: Source and amount of carbohydrate affect postprandial glucose and insulin in normal subjects [non-randomized study; weak evidence] ↩
Journal of Insulin Resistance 2016: It is the glycaemic response to, not the carbohydrate content of food that maters in diabetes and obesity: The glycaemic index revisited [overview article; ungraded] ↩
Point of Care 2017: Type 1 diabetes – a clinical perspective [overview article; ungraded] ↩
Diabetologia 2005: Symptoms, signs and complications in newly diagnosed type 2 diabetic patients, and their relationship to glycaemia, blood pressure and weight [observational study; very weak evidence] ↩
Social Science and Medicine 2019: “Wasting away”: diabetes, food insecurity, and medical insecurity in the Somali region of Ethiopia [observational study; very weak evidence] ↩
Plastic and Reconstructive Surgery 2013:The role of chronic and perioperative glucose management in high-risk surgical closures: a case for tighter glycemic control [observational study with OR >4; weak evidence]
The Journal of Investigative Dermatology 2012: Hemoglobin A1c is a predictor of healing rate in diabetic wounds[observational study; very weak evidence] ↩
Journal of Surgical Research 2016: The effect of local hyperglycemia on skin cells in vitro and on wound healing in euglycemic rats [animal study; very weak evidence]
Diabetes 2013: High-glucose environment enhanced oxidative stress and increased interleukin-8 secretion from keratinocytes: new insights into impaired diabetic wound healing [animal study; very weak evidence] ↩
World Journal of Diabetes 2015: Peripheral artery disease in patients with diabetes: Epidemiology, mechanisms, and outcomes [overview article; ungraded] ↩
Research 2014: Diabetes mellitus and refractive changes: analysis of three cases and review of the literature [case reports and literature review; very weak evidence] ↩
Journal Francais d’Ophtalmologie 2018: Oculomotor palsy in diabetics [retrospective study; very weak evidence] ↩
Diabetologia 2005: Symptoms, signs and complications in newly diagnosed type 2 diabetic patients, and their relationship to glycaemia, blood pressure and weight [observational study; very weak evidence] ↩
Clinical Therapeutics 2018: Diabetic Peripheral Neuropathy: Epidemiology, Diagnosis, and Pharmacotherapy [overview article; ungraded] ↩
These numbers are higher than what other studies report, but note that 29% of the control group also had neuropathy.
Diabetes Care 2015: Peripheral neuropathy and nerve dysfunction in individuals at high risk for type 2 diabetes: the PROMISE cohort [observational study; very weak evidence] ↩
Pain Medicine 2009: Neuropathic pain in diabetes, prediabetes and normal glucose tolerance: the MONICA/KORA Augsburg Surveys S2 and S3 [observational study; very weak evidence] ↩
Journal of Family Medicine and Primary Care 2017: Acanthosis nigricans: a screening test for insulin resistance – an important risk factor for diabetes mellitus type-2 [observational study; very weak evidence] ↩
Endocrine Practice 2004: Prevalence of acanthosis nigricans in newly-diagnosed type 2 diabetes [observational study; very weak evidence] ↩
Diabetology & Metabolic Syndrome 2017: Skin disorders in diabetes mellitus: an epidemiology and pathophysiology review [overview article; ungraded] ↩
Diabetology & Metabolic Syndrome 2017: Skin disorders in diabetes mellitus: an epidemiology and pathophysiology review [overview article; ungraded] ↩
Diabetes, Metabolic Syndrome and Obesity 2015: Urinary tract infections in patients with type 2 diabetes mellitus: review of prevalence, diagnosis, and management [overview article; ungraded]
Journal of Clinical Medicine 2019: Candida sp. Infections in patients with diabetes mellitus [overview article; ungraded]
Clinical Focus: Diabetes and Concomitant Disorders 2013: Genital mycotic infections in patients with diabetes [overview article; ungraded] ↩
Diabetic Medicine 2017: High prevalence of erectile dysfunction in diabetes: a systematic review and meta-analysis of 145 studies [observational study with hazard ratio > 2; weak evidence]
International Journal of Impotence Research 2017: Erectile dysfunction in young men with type 1 diabetes [observational study with hazard ratio > 2; weak evidence] ↩
The European Journal of Clinical Nutrition 2017: The interpretation and effect of a low-carbohydrate diet in the management of type 2 diabetes: a systematic review and meta-analysis of randomised controlled trials [strong evidence]
Frontiers in Endocrinology 2019: Long-term effects of a novel continuous remote care intervention including nutritional ketosis for the management of type 2 diabetes: a 2-year non-randomized clinical trial [weak evidence]
The American Journal of Clinical Nutrition 2018: Effects of low-carbohydrate- compared with low-fat-diet interventions on metabolic control in people with type 2 diabetes: a systematic review including GRADE assessments [strong evidence for some benefits of a low-carb diet]
Diabetes Care 2019: Nutrition therapy for adults with diabetes or prediabetes: a consensus report by the American Diabetes Association [overview article, ungraded; the ADA now endorses low-carb diets as one option for type 2 diabetes treatment] ↩
Some disagree with the use of the word “reverse” when it comes to type 2 diabetes. The concern is that it implies the disease is completely gone, never to return. At Diet Doctor, we use the term “reverse” to indicate that blood sugar levels are no longer in the diabetic range without the use of medications. However, we acknowledge that high glucose levels will likely recur if a patient goes back to their prior high-carb eating habits. Therefore, “reverse” does not imply a forever cure. ↩
Diabetes, Obesity & Metabolism 2019: Low versus high carbohydrate diet in type 1 diabetes: A 12-week randomized open-label crossover study [moderate evidence]
Asia Pacific Journal of Clinical Nutrition 2016: A randomised trial of the feasibility of a low carbohydrate diet vs standard carbohydrate counting in adults with type 1 diabetes taking body weight into account [moderate evidence] ↩















