Starting low carb or keto with diabetes medications
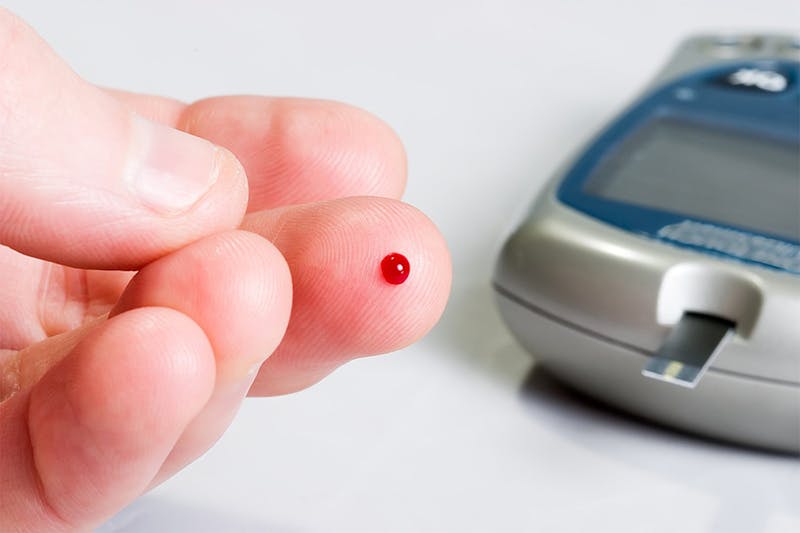
For instance, we want you to know that it’s very important to adjust diabetes medications when starting a low-carb diet. In particular, insulin doses may need to be lowered to avoid low blood sugar, and SGLT-2 inhibitors may need to be discontinued (see below).
We want you to discuss any changes in medication and lifestyle with your doctor before making any such changes. Full disclaimer
So you have diabetes and want to try eating low carb or keto? Good for you! Making these dietary changes has the potential to reverse type 2 diabetes.1 Or, if you have type 1 diabetes, doing so could dramatically improve your blood sugar control.2
However, you need to know what you are doing, and you need to communicate frequently with your healthcare team. Once you start eating low carb you will likely have to lower your insulin doses as well as the doses of other diabetes medications, frequently by quite a lot.3
Avoiding the carbohydrates that raise your blood sugar decreases your need for medication to lower it. Taking the same dose of insulin or insulin-stimulating oral medication as you did prior to adopting a low-carb diet might result in low blood sugar, something that can be dangerous.
You need to test your blood sugar frequently when starting this diet and adjust your medication accordingly. This should always be done with the assistance of a physician or other health professional with expertise in diabetes (find a low-carb doctor).
No drugs
If you have diabetes and you’re treated by diet alone, there is an extremely low risk of low blood sugar on low carb. You can get started right away.
Insulin-treated type 2 diabetes
As a general rule, you will need to lower your doses when starting a strict low-carb diet.4
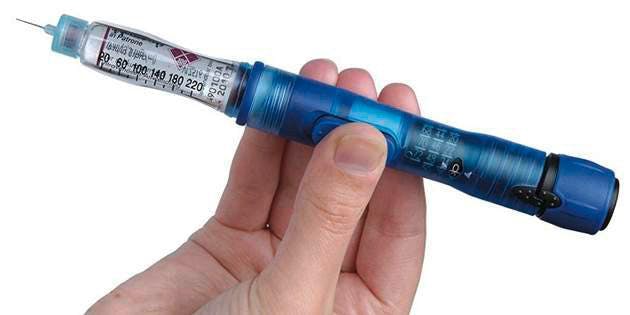


Work with your doctor to find the right initial reduction. Many find they need to reduce long acting insulin between 30 and 50%.5 If you take intermediate- or long-acting insulin once or twice daily, consider reducing both doses by the same proportion. If you are on a basal-bolus regimen (taking fast-acting insulin before meals, and long-acting insulin once or twice a day), you may want to reduce your mealtime doses more than your basal. This careful experimentation should be done in conjunction with your healthcare provider.
If you remain low carb, it is possible you will be able to stop mealtime insulin altogether. If your blood sugar levels continue to drop off the mealtime insulin, you can then begin to more aggressively reduce your long-acting insulin. As blood sugars stabilize in the normal range, you may be able to continue weaning the insulin, as long as glucose levels continue to be normal.6 Many people on a low carb diet are able to come off insulin completely.7
Note that many physicians feel it is safer to decrease insulin doses by too much rather than not enough. This is because taking too much insulin can result in a low blood sugar level, which has the potential to be acutely dangerous. On the other hand, having slightly high blood sugars for short periods of time is usually not going to have major health consequences.8
In addition, frequent low blood sugars lead to eating or drinking glucose or another form of rapid-acting carbohydrate in order to raise your glucose to a safe level. These extra calories may very well thwart your efforts at weight loss.
Insulin in type 1 diabetes
Much of the above advice about insulin also applies to people with type 1 diabetes, with the critical difference that people with type 1 will not be able to discontinue insulin entirely. Nonetheless, a low-carb, high-fat diet can be fantastic for empowering people with type 1 diabetes to smooth out their wide swings in blood sugar.910
However, eating low carb with type 1 diabetes requires even greater attention to blood sugar levels and insulin adjustment, and an even closer working relationship with your healthcare team.
Many people with type 1 diabetes use an insulin to carbohydrate ratio (ICR) to calculate their mealtime insulin doses. If using an ICR while eating a low-carb diet, you may continue to give the same ratio of insulin to the carbohydrates you eat. But, as you eat fewer carbs, you will be injecting less insulin overall.
In some cases, the amount of insulin required for meals will not decrease as much as would be expected for the lower carb intake; this is presumably due to the potential of higher protein intakes to increase gluconeogenesis (the production of “new sugar” by the liver).11 In other cases, insulin doses will drop more than expected, as some people will lose weight on a low-carb diet, becoming more insulin sensitive in the process.
People who use relatively fixed mealtime doses of insulin, or those on premixed insulin twice daily, should use a similar approach to those with type 2 diabetes. Again, the critical difference is that people with type 1 diabetes will always need some insulin, even on a very low-carbohydrate diet.
It is important to be aware that a diet with less than 50 grams of carbs each day can lead to ketosis, a normal physiological state that results from the body burning fat for energy. This should not be confused with ketoacidosis, a dangerous complication of type 1 diabetes that can occur when there is insufficient insulin.12
Because people with type 1 diabetes are at risk of progressing from physiologic ketosis to dangerous ketoacidosis, we recommend that they start with a more liberal low-carb diet, containing at least 50 grams of carbs per day.13 If you wish, you can eventually begin to reduce your carb intake to 30-40 grams of carbs per day, while working closely with your healthcare team and carefully monitoring your ketone levels.
We do not recommend starting a ketogenic low-carb diet (below 20 grams a day) unless you’re certain of how to manage this risk and are working closely with a very experienced healthcare practitioner. You have to be able to test your ketones often, using extra care if you feel even slightly ill, practice intermittent fasting, or have been exercising.14
Type 1 diabetes – how to control your blood sugar with fewer carbs
Insulin-releasing pills
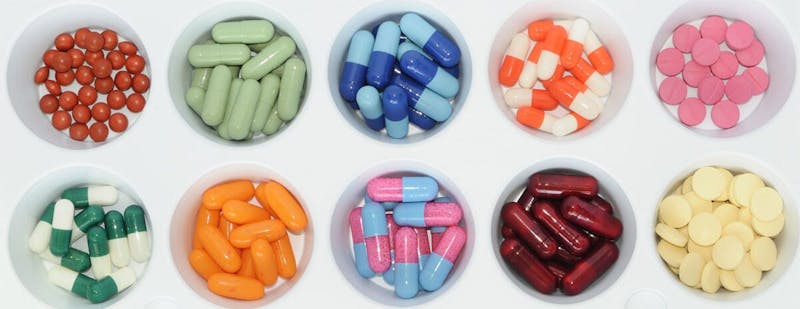



Some pills for type 2 diabetes work by directly stimulating the pancreas to produce more insulin. These medications increase the risk of low blood sugar on a low-carb diet.
The most common examples of these pills would be in the class known as sulfonylureas (e.g. glimepiride, gliclazide, glipizide, glibenclamide, glyburide, tolbutamide, etc.), while the class known as meglitinides (e.g. repaglinide and nateglinide) is used less often.
You will need to reduce the dose or stop these drugs when starting a low-carb diet in order to avoid low blood sugar levels.15 We recommend you discuss this with your doctor before starting a low-carb diet.
Metformin
Individuals with type 2 diabetes can can safely take metformin on a low-carb diet. There is a very low risk of low blood sugar from taking metformin.16
GLP-1 agonists and DPP-4 inhibitors
GLP-1 agonists typically have generic names ending in -tide like semaglutide, liraglutide, or exenatide. DPP-4 inhibitors typically have generic names ending in -gliptin like sitagliptin or linagliptin.
These drugs should rarely lead to low blood sugar on a low-carb diet, by themselves.17 But be observant, check your blood sugar often, and discuss changes with your doctor as needed.
SGLT-2 inhibitors
SGLT-2 inhibitors have generic names ending in -gliflozin, like canagliflozin, empagliflozin, and dapagliflozin. These drugs lower blood sugar by causing the kidneys to excrete more glucose into the urine. However, they can increase the risk of a dangerous condition called euglycemic ketoacidosis.18
The risk of euglycemic ketoacidosis may also be increased by a strict low-carb diet.19 It is therefore advised to stop SGLT-2 inhibitors before starting a strict low-carb diet, which should be discussed with your doctor.
It’s worth noting that when ketoacidosis occurs while taking an SGLT-2 inhibitor, the blood sugar level is not necessarily high, making it harder to detect.20
If you get symptoms of ketoacidosis – extreme thirst, nausea, vomiting, stomach pain, confusion, etc. – you should stop the medication and contact a doctor immediately.
Learn more
More
A keto (strict low-carb) diet for beginners
Low carb for doctors
Are you a doctor or do you know one? Here’s our low carb for doctors resource, with information on how to safely handle medications on a low-carb diet:
More resources
Did you enjoy this guide?
We hope so. We want to take this opportunity to mention that Diet Doctor takes no money from ads, industry or product sales. Our revenues come solely from members who want to support our purpose of empowering people everywhere to dramatically improve their health.
Will you consider joining us as a member as we pursue our mission to make low carb simple?
Starting low carb or keto with diabetes medications - the evidence
This guide is written by Dr. Andreas Eenfeldt, MD and was last updated on June 17, 2022. It was medically reviewed by Dr. Michael Tamber, MD on March 7, 2022.
The guide contains scientific references. You can find these in the notes throughout the text, and click the links to read the peer-reviewed scientific papers. When appropriate we include a grading of the strength of the evidence, with a link to our policy on this. Our evidence-based guides are updated at least once per year to reflect and reference the latest science on the topic.
All our evidence-based health guides are written or reviewed by medical doctors who are experts on the topic. To stay unbiased we show no ads, sell no physical products, and take no money from the industry. We're fully funded by the people, via an optional membership. Most information at Diet Doctor is free forever.
Read more about our policies and work with evidence-based guides, nutritional controversies, our editorial team, and our medical review board.
Should you find any inaccuracy in this guide, please email andreas@dietdoctor.com.
Some disagree with the use of the word “reverse” when it comes to type 2 diabetes. The concern is that it implies the disease is completely gone, never to return. At Diet Doctor, we use the term “reverse” to indicate that blood sugar levels are no longer in the diabetic range without the use of medications. However, we acknowledge that high glucose levels will likely recur if a patient goes back to their prior high-carb eating habits. Therefore, “reverse” does not imply a forever cure. ↩
Type 2 diabetes:
Nutrients 2019: Reversing type 2 diabetes: a narrative review of the evidence [overview article; ungraded]
Diabetes Research and Clinical Practice 2018: Effect of dietary carbohydrate restriction on glycemic control in adults with diabetes: a systematic review and meta-analysis [strong evidence]
Type 1 diabetes:
Diabetes, Obesity and Metabolism 2019: Low versus high carbohydrate diet in type 1 diabetes: a 12-week randomized open-label crossover study [moderate evidence]
Asia Pacific Journal of Clinical Nutrition 2016: A randomised trial of the feasibility of a low carbohydrate diet vs standard carbohydrate counting in adults with type 1 diabetes taking body weight into account [moderate evidence]
↩This is true for people with type 1 diabetes as well as those with type 2 who take mealtime insulin. It is also true for many oral medications that lower blood sugar.
Diabetes, Obesity and Metabolism 2014: Two diets with different haemoglobin A1c and antiglycaemic medication effects despite similar weight loss in type 2 diabetes [randomized trial; moderate evidence]
Diabetes Therapy 2018: Effectiveness and safety of a novel care model for the management of type 2 diabetes at 1 year: an open-label, non-randomized, controlled study [weak evidence]
Upsala Journal of Medical Sciences 2005: A low-carbohydrate diet in type 1 diabetes: clinical experience — a brief report [weak evidence]
↩How much you need to reduce your insulin dosage depends on several factors, including carb intake and blood sugar control before starting a low-carb diet. Generally speaking, the lower your average blood sugars before you start eating low carb, the more you will need to reduce insulin when lowering your carb intake. Similarly, the higher your carb intake before switching to low carb, potentially the greater the need for reducing insulin.
Nutrition & Metabolism 2008: The effect of a low-carbohydrate, ketogenic diet versus a low-glycemic index diet on glycemic control in type 2 diabetes mellitus [randomized trial; moderate evidence]
Nutrition & Metabolism 2005 : A low-carbohydrate, ketogenic diet to treat type 2 diabetes [non-randomized trial; weak evidence]
↩British Journal of General Practice 2019: Adapting diabetes medication for low carbohydrate management of type 2 diabetes: a practical guide. [overview article; ungraded] ↩
There is no universal agreement of what defines stable or acceptable blood sugar levels in this scenario. The details will vary depending on an individual’s concern about hypoglycemia versus their interest in strict glucose control. Appropriate targets should be discussed with your healthcare team. ↩
Diabetes Therapy 2018: Effectiveness and safety of a novel care model for the management of type 2 diabetes at 1 year: an open-label, non-randomized, controlled study [weak evidence] ↩
This is based on consistent clinical experience of low-carb practitioners. [weak evidence] ↩
You can hear about this in more detail in our podcast interview with type 1 diabetes low-carb expert Dr. Jake Kushner. ↩
In one study, people with type 1 diabetes reported 82% less hypoglycemia at the one-year mark of following a low-carbohydrate diet providing about 75 grams of carbs per day:
Upsala Journal of Medical Sciences 2005: A low-carbohydrate diet in type 1 diabetes: clinical experience — a brief report [weak evidence]
Other studies have also shown that lower carb intake can result in significantly fewer hypoglycemic episodes in those with type 1 diabetes:
Diabetes, Obesity and Metabolism 2019: Low versus high carbohydrate diet in type 1 diabetes: a 12-week randomized open-label crossover study [moderate evidence]
Diabetes, Obesity and Metabolism 2017: Short-term effects of a low carbohydrate diet on glycaemic variables and cardiovascular risk markers in patients with type 1 diabetes: a randomized open-label crossover trial [moderate evidence]
↩Asia Pacific Journal of Clinical Nutrition 2016: A randomised trial of the feasibility of a low carbohydrate diet vs standard carbohydrate counting in adults with type 1 diabetes taking body weight into account [moderate evidence] ↩
Nutrition Bulletin 2011: Ketosis, ketoacidosis and very-low-calorie diets: Putting the record straight [overview article; ungraded] ↩
This is based on consistent clinical experience of low-carb practitioners. [weak evidence] ↩
All of these factors increase ketone production in the liver. In people who don’t have diabetes, the pancreas responds to rising ketone levels by releasing more insulin, which signals the liver to produce fewer ketones. Because this feedback loop is absent in those with type 1 diabetes, higher ketone levels may lead to diabetic ketoacidosis unless sufficient insulin is taken.
Diabetes Metabolism Reviews 1989: Ketone body production and disposal: effects of fasting, diabetes, and exercise [overview article; ungraded]
Diabetes Metabolism Research & Reviews 1999: Ketone bodies: a review of physiology, pathophysiology and application of monitoring to diabetes[overview article; ungraded]
↩In low-carb studies, sulfonylurea medications often need to be discontinued within just a few days due to rapid improvement in blood sugar levels.
Nutrition and Diabetes 2017: Twelve-month outcomes of a randomized trial of a moderate-carbohydrate versus very low-carbohydrate diet in overweight adults with type 2 diabetes mellitus or prediabetes [moderate evidence]
Diabetes, Obesity and Metabolism 2014: Two diets with different haemoglobin A1c and antiglycaemic medication effects despite similar weight loss in type 2 diabetes [randomized trial; moderate evidence]
Nutrition & Metabolism 2005 : A low-carbohydrate, ketogenic diet to treat type 2 diabetes [non-randomized trial; weak evidence]
↩Metformin improves insulin sensitivity and decreases the amount of sugar released by your liver but does not increase the amount of insulin released by your pancreas. Therefore, your blood sugar remains stable and doesn’t drop too low, no matter how few carbs you eat.
Endokrynologia Polska 2017: Metformin – a new old drug [overview article; ungraded]
Many ketogenic diet trials, including the trials by Virta Health, kept patients on metformin without any complications.
Diabetes Therapy 2018: Effectiveness and safety of a novel care model for the management of type 2 diabetes at 1 year: an open-label, non-randomized, controlled study [weak evidence]
↩Unlike sulfonylureas, GLP-1 receptor agonists and DPP-4 inhibitors predominantly lower blood sugar only when it is elevated, resulting in a very low risk of hypoglycemia.
American Health and Drug Benefits 2017: Overview of glucagon-like peptide-1 receptor agonists for the treatment of patients with type 2 diabetes [overview article; ungraded]
Acta Diabetologica 2019: Ten years of experience with DPP-4 inhibitors for the treatment of type 2 diabetes mellitus [overview article; ungraded]
↩The Journal of Clinical Endocrinology and Metabolism 2019: SGLT2 inhibitors increase the risk of diabetic ketoacidosis developing in the community and during hospital admission [retrospective cohort study; very weak evidence]
↩Low-carbohydrate diets have been identified as a contributing factor to diabetic ketoacidosis in those taking SGLT-2 inhibitors.
Clinical Therapeutics 2016: SGLT2 inhibitor-associated diabetic ketoacidosis: clinical review and recommendations for prevention and diagnosis [overview article; ungraded]
↩Although relatively rare, diabetic ketoacidosis without elevated blood sugar (referred to as euglycemic DKA) has been found to occur in both people with type 1 and type 2 diabetes who take SGLT-2 inhibitors.
Diabetes Care 2019: International consensus on risk management of diabetic ketoacidosis in patients with type 1 diabetes treated with sodium-glucose cotransporter (SGLT) inhibitors [overview article; ungraded]
Clinical Therapeutics 2016: SGLT2 inhibitor-associated diabetic ketoacidosis: clinical review and recommendations for prevention and diagnosis [overview article; ungraded]
↩



















