Gout and low carb
 Do low-carb or keto diets high in meat cause gout? This is an especially important question to ask, given that the conventional advice for gout-sufferers has long been to avoid excessive meat and seafood consumption. In this guide, we will explore the evidence on this topic, proving that there is significantly more nuance than previously appreciated.
Do low-carb or keto diets high in meat cause gout? This is an especially important question to ask, given that the conventional advice for gout-sufferers has long been to avoid excessive meat and seafood consumption. In this guide, we will explore the evidence on this topic, proving that there is significantly more nuance than previously appreciated.
First, it’s necessary to recognize that a low-carb diet is not necessarily high in meat.1 However, low-carb diets that are high in meat are markedly different from a meat-heavy, standard American diet.2
Second, it is worth emphasizing that all low-carb diets should have negligible amounts of sugar and refined carbohydrate. This is critical because there is a growing body of evidence suggesting a strong association between sugar intake and the risk of gout. If this relationship eventually proves to be a causal one, then low-carb diets would be considered a therapeutic tool for reducing the risk of gout.3
Keep reading to learn the definition of gout, how to avoid it, and how a low-carb diet may affect it.
What is gout?
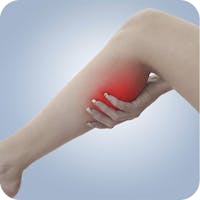
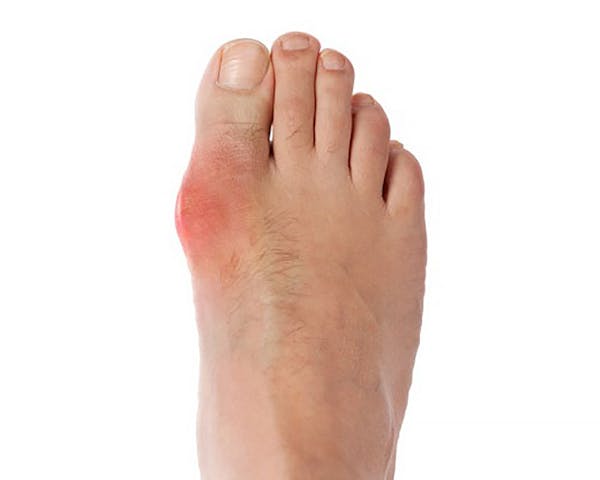
Gout is a sudden and painful inflammation of a joint, most often at the base of the big toe (see image). It may also affect other joints, like heels, knees, wrists and finger joints.
The cause of gout is elevated levels of uric acid in the blood, resulting in crystals depositing in the affected joint.
Gout is more common in people who are overweight and have metabolic syndrome. Given the increasing prevalence of those conditions in recent decades, gout now affects about 6% of adult men and 2% of women (it’s even more common in older people).4
Meat and gout
Gout has often been blamed on excessive consumption of meat. This is because the uric acid that causes gout is a breakdown product of purines – the building blocks of protein that are highly concentrated in meat.
Some weak observational studies, especially those in the United states, show an association between meat intake and elevated uric acid levels.5 Others, such as one in Taiwan, show no such association.6
Why the difference?
We don’t know for sure, but one proposed explanation is that a higher prevalence of metabolic syndrome or consumption of sugar may account for such geographic differences. If true, this could suggest that other components of diet may matter more than the consumption of meat itself.
It’s also important to consider that, as with all nutritional epidemiology studies, it is quite difficult to separate the effects of meat on gout risk from those of refined grains or alcohol.
Further, there is a real concern for healthy user bias in these studies, in that those consuming large amounts of meat as part of a typical Western diet may engage in other unhealthy behaviors that increase the risk of gout.7
Therefore, it’s important to note that epidemiology studies cannot prove that meat directly increases the risk of gout.
Further, we must acknowledge that nutrition research often yields conflicting results for the same topic, like one study showing that vegans had higher uric acid levels than meat eaters and fish eaters.8
Does this mean that vegans have the highest risk for gout attacks? No, we cannot conclude that based on these data, and the bottom line is that we must consider the results of nutritional epidemiology studies with a healthy dose of skepticism.
Sugar and gout
As there is a very strong connection among elevated uric acid levels, gout, obesity, type 2 diabetes and metabolic syndrome, it’s possible that they are all associated with and exacerbated by the same thing: sugar and other refined carbohydrates.9
In fact, there is a striking history of gout suddenly becoming common in populations just as sugar consumption started to rise sharply (e.g. in Britain during the eighteenth century, paralleling the birth of the country’s sugar industry).10
Mechanistically, there are clear explanations for the relationship between sugar intake and uric acid levels. Fructose (found in sweetened beverages, among other things) is well-known to directly increase blood uric acid levels.11 In addition, elevated blood insulin levels – associated with a diet high in sugar and refined carbs – have been shown to increase uric acid levels, likely by decreasing the excretion of uric acid by the kidneys.12
Further, observational studies consistently show a correlation between fructose consumption and an increased risk of gout.13 Although these types of studies cannot prove that fructose causes gout, we believe that the combination of mechanistic and consistent observational data makes a compelling case for avoiding fructose to decrease the risk of gout.
Low carb, uric acid and gout
Short term studies show a temporary rise in uric acid during the first few weeks when starting a strict low-carb (i.e. keto) diet. This effect seems to disappear after about six weeks, with uric acid returning to baseline or even lower.14
After dozens of high-quality studies comparing low-carb diets to other diets, there seem to be none noticing any obvious difference in the risk of gout, although no study has specifically focused on this question.
Doctors regularly treating patients with low-carb diets do not notice a sharp increase in gout episodes, even during the initial time period.17 If there exists an increase in risk during the first few weeks, it is likely small.
How to avoid gout
Here’s how to avoid gout long term, using only lifestyle modifications:
- Minimize intake of sugar.18
- Reduce intake of alcohol. Particularly avoid beer and other high-carb alcoholic drinks.19
- Lose excess weight and reverse metabolic syndrome. Low carb is a good treatment, as is intermittent fasting.20
- Avoid dehydration.21
As a bonus, these lifestyle modifications have many other positive effects on weight and health.
Given that there may be a temporary rise in uric acid during the first few weeks on a strict low carb diet, some recommend that people who’ve previously had troublesome gout attacks may want to consider using the drug allopurinol while starting low carb.
However, rheumatologist Dr. Edward Skol from Scripps Clinic warns against temporary use of allopurinol for this purpose; it is known to initially increase the risk of an acute attack when started (and when stopped) without the use of additional anti-gout medication. This is supported by the American College of Rheumatology official guidelines, which strongly recommend only starting allopurinol in conjunction with a medication like colchicine or ibuprofen to decrease this initial risk.22
In Dr. Skol’s practice, if medication is desired to prevent gout attacks at the start of a low-carb diet, he most commonly uses just colchicine or ibuprofen without allopurinol. He also summarizes, “The best advice is probably just avoiding dehydration when starting a ketogenic diet.”23
Meat or no meat?
Avoiding meat should not be necessary when it comes to gout prevention, especially when otherwise following a low-carb diet.
Furthermore, please note that a low-carb diet does not have to be especially high in meat anyway. Multiple other foods exist to achieve your protein needs.
A well-formulated low-carb diet that reduced sugars and refined carbohydrates could potentially reduce the risk of gout long term.24
More low-carb side effects & how to cure them
Common early issues
Less common issues
Low-carb myths
More
Improve this page
Do you have any suggestion – big or small – to improve this page?
Anything that you’d like added or changed? Any other problems you’d like to see addressed?
E-mail me at andreas@dietdoctor.com.
Gout and low carb - the evidence
This guide is written by Dr. Andreas Eenfeldt, MD and was last updated on August 9, 2022. It was medically reviewed by Dr. Michael Tamber, MD on August 9, 2022.
The guide contains scientific references. You can find these in the notes throughout the text, and click the links to read the peer-reviewed scientific papers. When appropriate we include a grading of the strength of the evidence, with a link to our policy on this. Our evidence-based guides are updated at least once per year to reflect and reference the latest science on the topic.
All our evidence-based health guides are written or reviewed by medical doctors who are experts on the topic. To stay unbiased we show no ads, sell no physical products, and take no money from the industry. We're fully funded by the people, via an optional membership. Most information at Diet Doctor is free forever.
Read more about our policies and work with evidence-based guides, nutritional controversies, our editorial team, and our medical review board.
Should you find any inaccuracy in this guide, please email andreas@dietdoctor.com.
It is possible to eat either a vegan or vegetarian low-carb diet:
Very low-carb diets studied in the literature usually include less than 30 grams of carbohydrates per day, while moderate to liberal low-carb trials may include up to 50 or 100 grams of carbs, respectively.
On the other hand, observational studies of the standard American diet estimate an average intake of 250 grams of total carbs/day, with 210 grams of that considered “low quality.”
JAMA 2019: Trends in dietary carbohydrate, protein, and fat intake and diet quality among US adults, 1999-2016 [nutritional epidemiology study, very weak evidence]
↩Observational studies have found an association between sugar intake and risk of gout. More evidence is needed to show a cause and effect relationship.
BMJ Open 2016: Fructose intake and risk of gout and hyperuricemia: a systematic review and meta-analysis of prospective cohort studies [meta-analysis of nutritional epidemiology studies; very weak evidence]
Seminars in Nephrology 2011: The epidemiology of uric acid and fructose [nutritional epidemiology study; very weak evidence] ↩
Arthritis & Rheumatology 2011: Prevalence of gout and hyperuricemia in the US general population: The National Health and Nutrition Examination Survey 2007–2008 ↩
Arthritis and Rheumatism 2005: Intake of purine-rich foods, protein, and dairy products and relationship to serum levels of uric acid: the Third National Health and Nutrition Examination Survey. [observational study, weak evidence] ↩
Seminars in Arthritis and Rheumatism 2008: Dietary factors associated with hyperuricemia in adults. [observational study, weak evidence] ↩
The following study showed a very weak association between certain sources of animal protein intake and the risk of gout. However, those who had gout also drank more alcohol, were more likely to have hypertension, and ate more total calories.
Arthritis and Rheumatology 2015: Food sources of protein and risk of incident gout in the Singapore Chinese health study [nutritional epidemiology study; very weak evidence] ↩
PLOS One 2013: Serum uric acid concentrations in meat eaters, fish eaters, vegetarians and vegans: A cross-sectional analysis in the EPIC-Oxford Cohort [nutritional epidemiology study, very weak evidence] ↩
American Journal of INternal Medicine 2007: Prevalence of the metabolic syndrome in individuals with hyperuricemia [observational study, weak evidence]
Arthritis and Rheumatology 2015: Risk of incident diabetes in patients with gout: a cohort study [observational study, weak evidence] ↩
Rheumatology 2013: Sack and sugar, and the aetiology of gout in England between 1650 and 1900 [overview article; ungraded] ↩
Lancet 1970: Fructose-induced hyperuricaemia.[non-controlled study; weak evidence] ↩
Journal of Clinical and Diagnostic Research 2013: Correlation of the serum insulin and the serum uric acid levels with the glycated haemoglobin levels in the patients of type 2 diabetes mellitus [observational study, weak evidence] ↩
This meta-analysis of observational studies showed that fructose and alcohol consumption correlated the strongest with risk of gout – stronger than meat and seafood consumption.
Asia Pacifica Journal of Clinical Nutrition 2018: Dietary factors and risk of gout and hyperuricemia: a meta-analysis and systematic review [meta-analysis with HR>2 for association of fructose and alcohol with gout; weak evidence]
BMJ Open 2016: Fructose intake and risk of gout and hyperuricemia: a systematic review and meta-analysis of prospective cohort studies[meta-analysis of observational studies; weak evidence]
BMJ 2008: Soft drinks, fructose consumption, and the risk of gout in men: prospective cohort study. [observational study, weak evidence] ↩
Nutrition 2012: Effect of low-calorie versus low-carbohydrate ketogenic diet in type 2 diabetes. [randomized trial; moderate evidence] ↩
NEJM 2003: A Low-Carbohydrate as Compared with a Low-Fat Diet in Severe Obesity [randomized trial; moderate evidence]
Obesity reviews 2012: Systematic review and meta-analysis of clinical trials of the effects of low carbohydrate diets on cardiovascular risk factors [strong evidence] ↩
American Collage of Rheumatology 2014: High-Protein Diet (Atkins Diet) and Uric Acid Response [non-controlled study; weak evidence] ↩
This is based on clinical experience of low-carb practitioners and was unanimously agreed upon by our low-carb expert panel. You can learn more about our panel here [weak evidence]. ↩
Sugar is likely worse than other carbohydrates because of the potency of fructose in raising uric acid.
This study showed lowering the glycemic index of dietary carbohydrates improved uric acid levels:
Arthritis and Rheumatology 2017: Effects of lowering glycemic index of dietary carbohydrate on plasma uric acid: The OmniCarb Randomized Clinical Trial[randomized trial; moderate evidence] ↩
Beer not only contains alcohol, but also rapidly digestible carbs, raising insulin and thus lowering excretion of uric acid. Of less importance, beer also contains purines.
This study showed most types of alcohol, even in moderate amounts, increased risk of gout. However, it is likely that none of the participants were on a low-carb diet.
American Journal or Medicine 2015 Alcohol quantity and type on risk of recurrent gout attacks: An internet-based case-crossover study [anecdotal report; very weak evidence]
If you want to drink alcohol, ideally choose options low in carbohydrates. This may still raise uric acid levels and the risk of gout, but possibly by less (this is not based on clinical evidence but rather on mechanistic thinking):
↩The American Journal of Medicine: Update on Importance of Diet in Gout [overview article; ungraded] ↩
PLoS One 2017: Triggers of acute attacks of gout, does age of gout onset matter? A primary care based cross-sectional study [observational study, weak evidence] ↩
Arthritis Care Research 2020:
2020 American College of Rheumatology guideline for the management of gout [overview article; ungraded] ↩This is based on clinical experience. [weak evidence] ↩
Although we are not aware of any long term studies specifically looking at low-carb and gout, it makes empiric sense that reducing sugar intake and improving metabolic syndrome would reduce the future risk of gout. ↩