Can low carb or keto help with gestational diabetes?
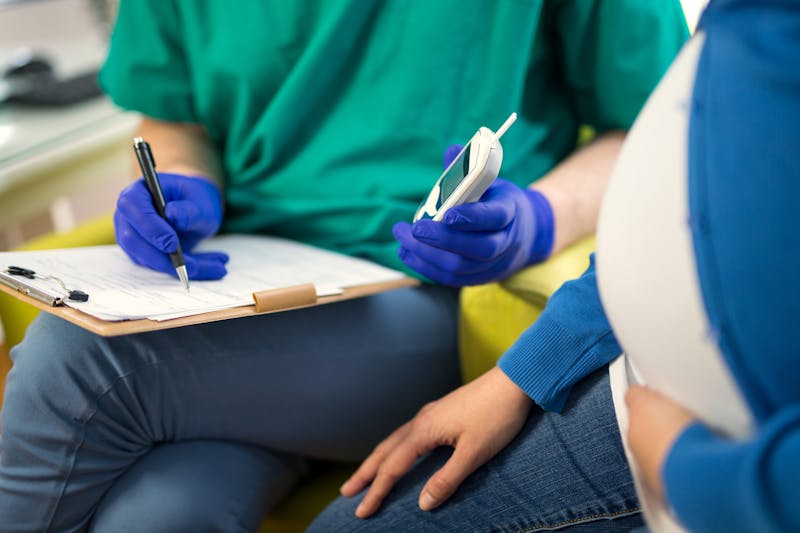
Diet Doctor is not stating that ketogenic diets have been scientifically proven to be safe in pregnancy. Unfortunately, it will be difficult — if not impossible — to obtain an adequate level of scientific evidence, given the ethical issue of performing these types of studies in pregnant women.
When Natalie Thompson Cooper was diagnosed with gestational diabetes in her first pregnancy, at age 28, she was very concerned. The condition, which affects at least one in seven pregnancies to as many as one in five, causes blood sugars to rise abnormally high, which is called hyperglycemia.3
Natalie knew hyperglycemia exposed her body tissues and her unborn daughter to high levels of glucose, putting both her and her fetus at risk for a wide range of potential complications, including miscarriage, birth defects, macrosomia (very large size), high blood pressure, pre-eclampsia, seizures, birth trauma, and higher rates of C-section and even stillbirth.4
Moreover, gestational diabetes (GD) — also called ‘carbohydrate intolerance of pregnancy’ — greatly increases the risk that the mother and her offspring will both face future health problems, such as much higher rates of eventual type 2 diabetes, metabolic conditions, and cardiovascular disease.5
Gestational diabetes is one of the most common and significant complications of pregnancy. Prenatal guidelines the world over recommend the routine screening of all pregnant women and then, if positive, strict management, starting with dietary therapy and moving on to insulin injections if that doesn’t work.6
However, to this day, what constitutes the best “dietary therapy” is hotly debated, with some researchers proposing a diet high in complex carbohydrates (60% carbs) and others lower carbohydrates (40% carbs).7
However, the recommended “lower carb” GD diet is still far higher than the under 20 grams per day of a strict low-carb or ketogenic diet. In fact, many guidelines for GD recommend women, on an ostensibly “lower-carb” diet, eat a minimum 175 grams of carbohydrate daily — an intake at which many women see their blood sugar rise to potentially unhealthy levels.8
She ate what they advised — bananas, whole grain toast, fruit, rice, steel cut oats — and was checking her blood sugar with a home monitor seven times a day. The results were always too high. Soon she was on four insulin injections a day, but still the GD was uncontrolled. She developed preeclampsia (high blood pressure and protein in her urine). Her daughter was born by C-section at 37 weeks, weighing 8 lbs (4 kg). “The diet did not help me AT ALL!”
Finding the ketogenic diet
Six years later — after failed fertility treatments for her PCOS, a miscarriage, and a successful adoption — Natalie discovered ketogenic eating. She lost 40 lbs (18 kg) in three months, which brought her weight down to 210 lbs (95 kg), helping her infertility and her PCOS symptoms. Much to her surprise, after six years of infertility, she was suddenly pregnant.




In the second pregnancy she developed GD, again, at 18 weeks. Her doctors and dietitian gave her exactly the same advice — carbs at every meal and at three snacks a day for a minimum daily requirement of 175 grams. This time Natalie just smiled and nodded but kept her carbs below 50 grams and monitored her blood sugar regularly with a home meter. She eventually needed insulin, but just one injection at bedtime. “It wasn’t perfect, but I was much more successful at keeping my blood sugars in check. There was no way I could eat the amount of carbs they recommended. If I did, my blood sugars would be way too high.”
Now, age 36, she is happily pregnant for the third time at 24 weeks.11 She has continued keto eating these past two years, resulting in a total weight loss of 95 lbs (43 kg) and a healthy pre-pregnancy weight of 155 lbs (70 kg). In June, at 18 weeks, she had a glucose tolerance test again to screen for GD. She drank a standardized solution with 50 grams of sugar and had her blood glucose checked one hour later. This time she passed with flying colors: her blood sugar was 85 mg/dl (4.7 mmol/l). “That is about as perfect as you can get!”12
Will she still develop GD later in this pregnancy? She doesn’t know, but she will do her utmost not to up her carb consumption and will monitor her blood sugars regularly. She has set the goal of under 50 grams of carbs per day and hopes to get down to 25 grams if possible. “I cannot believe that 175 grams of carbs is still being recommended for GD! It is insane.”13
Is the current advice based on solid science?




Nichols gives the same advice. She is the author of the 2015 book Real Food for Gestational Diabetes, offers an online gestational diabetes course and blogs at her web site.
Nichols has specialized in gestational diabetes for most of her career, initially with a California GD program called “Sweet Success,” which also recommended the minimum 175 grams of carbs daily. “It was always really disappointing to see how many of my prenatal clients would end up, as we say, ‘failing diet therapy’ and would have to go on insulin. It didn’t make sense to me why somebody with gestational diabetes, which translates as carbohydrate intolerance, would need such a high level of carbs,” said Nichols.
That experience set Nichols off digging into the historical literature to find out why 175 grams per day had become the minimum standard. “It turns out that this number is a best guess and not based in solid science. There is no evidence that eating fewer than 175 grams of carbohydrates is harmful.”15




Reproductive expert Dr. Michael Fox notes that in obstetrics training, doctors are taught that ketones in the urine represent starvation ketosis. This is often seen in hyperemesis patients (severe nausea and vomiting) and in patients who are not eating enough calories during pregnancy.
Dr. Fox believes that as long as pregnant women are eating frequently (at least every 3 hours) and consuming plenty of calories (about 2500 calories or more per day), ketones in the urine or blood is not an abnormal state and should be expected with a ketogenic approach.16
While pregnant women might get push-back from doctors not yet familiar with nutritional ketosis, one approach is to say, “I am following a ketogenic nutritional approach as I believe it is beneficial for my metabolic health, and this may result in ketones being detected in my urine. I would appreciate it if you could follow me during my pregnancy like you would anyone else, understanding that urine ketones are not necessarily a sign of trouble.”
While nutritional ketosis clearly appears to be safe in non-pregnant people, some doctors may continue to express concerns about a low-carb diet, given the lack of clarity in the medical literature regarding whether maternal ketones have any adverse effects on the developing baby.17
Nonetheless, Drs. Fox and Jovanovic, as well as Ms. Nichols, all say that pregnant women with GD can reduce their carbohydrates and not fear ketones in their urine as long as their blood sugars remain normal and they are eating enough calories from nutrient dense foods.
In extensive interviews for this post, these experts offered four practical tips for managing the risk of GD for all pregnant women, especially those at higher risk of GD, such as women with polycystic ovarian syndrome (PCOS), prediabetes, obesity, and previous GD in pregnancy.
Tip #1: Have early blood sugar tests to assess your risk
Women who go into pregnancy with pre-existing insulin resistance, or undiagnosed pre-diabetes, are much more likely to develop GD.18 In addition, the physiology of pregnancy naturally increases insulin resistance, potentially compounding the issue.
An HbA1c test — which measures the average blood sugar levels in the previous three months — taken prior to pregnancy or early in the first trimester can help identify women at risk in advance. Values greater than 5.7% may indicate prediabetes, and many doctors treat this the same as gestational diabetes. The higher the number, the higher your average blood sugar. A level of 5.9% or higher accurately predicates gestational diabetes 98.4% of the time.19 Note: HbA1C tests later in the pregnancy are less reliable because of rapid blood cell turnover and low iron stores.20
A fasting blood glucose prior to pregnancy or early in the first trimester can also help flag potential problems, if values are higher than 5.6 mmol/l (100 mg/dl), which is suggestive of prediabetes. Depending on your result, you may need to make blood sugar control a bigger priority. “Tackling it upfront can prevent blood sugar issues in the pregnancy and future complications,” Nichols said. Jovanovic agrees: “Waiting until 24 to 28 weeks to diagnosis GD means the fetus may have spent many weeks earlier in the pregnancy exposed to high blood sugars. You want to be on top of it early.”21
Tip #2: Self monitor with a home glucose monitor
Women at higher risk of GD, with a confirmed GD diagnosis, or who are interested in knowing about how their pregnancy and their diet is impacting their blood sugar, should consider getting a home glucose monitor. Times of the day to test are: a fasting blood glucose first thing in the morning and one to two hours after every meal or snack. Or even better, ask your doctor for a prescription for a continuous glucose monitor (CGM).22
Both note that if you have a couple of weeks showing normal blood sugar, you can keep eating the way you are eating. Just be aware that if your readings looked great in early pregnancy, you need to check again for a few weeks in the 24-28 week window since insulin resistance goes up later in pregnancy.24 Some people like Natalie Thompson Cooper have chosen to self-monitor their blood sugar regularly through their entire pregnancy.
Many types of home glucose monitors are available from your local pharmacy. Follow the instructions that come with your particular meter. In general, wash your hands with soap and water and dry well before testing. Do not use alcohol wipes as this may alter the result. Also, do not touch any food before testing, as this can raise the readings.
The general consensus is that you are aiming for the following results:25
- Fasting blood glucose less than 95 mg/dl (5.3 mmol/l).
- 1-hour post meal (postprandial) blood glucose less than 140 mg/dl (7.8 mmol/l)
- 2-hour post meal blood glucose less than 120 mg/dl (6.7 mmol/l)
Keep track of your daily blood glucose readings, the food you ate, and the exercise you did, either in a notebook or with an app or online tracker.
Tip #3: Understand the options for screening and diagnosis
Screening for GD typically happens in the first trimester for those at high risk (women with previous GD or PCOS) and at 24-28 weeks for all other pregnant women. The first test is typically the glucose challenge: drinking a standardized solution with 50 grams of sugar and having blood glucose tested one hour later.
It is well-known that people on low-carbohydrate diets are prone to false positive results when they have a glucose challenge. For this reason, women on low-carb diets who need to be screened for GD should consider raising their daily carbohydrate intake to above 150 grams a minimum of three days preceding a glucose challenge, although at least one study suggests it may take more than a week to fully adapt.26
Many women find the sugary drink can cause nausea, vomiting, dizziness, and headache. Studies have found eating 50 grams of sugar in 28 jelly beans or 10 sticks of a very popular (in North America) strawberry-flavored licorice candy, called “Twizzlers,” may be easier to tolerate, with fewer side effects, but still provide the same results.27




Women who fail the glucose challenge must then have a three-hour oral glucose tolerance test (OGTT) to confirm the GD diagnosis. That entails drinking twice the amount of sugar (100 grams) and having blood tested hourly over the following three hours.28
The International Association of Diabetes and Pregnancy Study Group (IADPSG) recommends — and many countries other than the United States use — a single screening test: the 2-hour, 75-gram glucose tolerance test.29
Nichols and Jovanovic believe that women can forgo the screening tests if they instead choose to track their blood sugar at home. “You can always decline the tests. You have that right. But you should be tracking your own sugars,” says Nichols. Jovanovic advises: “Just show [your doctors] your home blood sugars. That is all that matters.”30
Tip #4: Eat a nutrient-dense “whole-food” diet
The cover of Nichols book features two fried eggs with sliced avocado and cherry tomatoes — a low-carb high-fat meal. “It is the perfect breakfast, or any meal, for gestational diabetes,” she says. Her advice: eat nutrient-dense foods over empty calories.
“Some low-carb people are just living off fat bombs and bulletproof coffee. You need to have good, common sense with variety in your diet.” She recommends having protein like meat, fish, and eggs; snacks like nuts and seeds; and lots of vegetables with natural fats like olive oil or butter. Nichols suggests eating liver once or twice a week, to help ensure a good natural intake of vitamins, minerals, and antioxidants in your diet.
She further recommends avoiding all highly processed foods, added sugar, refined carbs, as well as high-glycemic fruit and fruit juices. If your blood sugar is still high, consider cutting out all fruit except berries. “You do not need to add in bread and cereals to have a healthy pregnancy,” says Nichols. Pay attention to how you feel, and monitor your blood sugars. “Some pregnant women may feel better eating slightly more carbs, but I think the majority of women with GD, and all pregnant women in general, do better with at least one-half to one-quarter the carbohydrates recommended in conventional nutrition guidelines (which is upwards of 65% of calories from carbohydrates).”31
Are gestational diabetes programs around the globe now registering that message and advising lower carb? Alas, not yet.
“What do you think would happen if I followed their advice?” asked Sarah incredulously, emailing the advice she received to Dr. Andreas Eenfeldt and the Diet Doctor team.
She believes that she’s likely been insulin resistant and prediabetic for years. She found the low-carb, high-fat diet and Diet Doctor five years ago. During this pregnancy, her third, she has been eating a more liberal low-carb diet, consuming more fruit than normal.
But now with the GD diagnosis, she is sticking to a lower-carb diet and monitoring her blood sugars regularly with a home meter, and she’s doing well. “Home monitoring is brilliant. I love doing it. I can see the impact of the foods I eat immediately,” says the math teacher. “I know if I followed the NHS dietary advice my blood sugar would get much, much worse.”
More
Is low carb safe during pregnancy?
Trying to conceive? Try the Better Baby Diet of beef, butter & bacon
Can low carb or keto help with gestational diabetes in pregnancy? - the evidence
This guide is written by Anne Mullens and was last updated on June 17, 2022. It was medically reviewed by Dr. Michael Tamber, MD on January 11, 2022.
The guide contains scientific references. You can find these in the notes throughout the text, and click the links to read the peer-reviewed scientific papers. When appropriate we include a grading of the strength of the evidence, with a link to our policy on this. Our evidence-based guides are updated at least once per year to reflect and reference the latest science on the topic.
All our evidence-based health guides are written or reviewed by medical doctors who are experts on the topic. To stay unbiased we show no ads, sell no physical products, and take no money from the industry. We're fully funded by the people, via an optional membership. Most information at Diet Doctor is free forever.
Read more about our policies and work with evidence-based guides, nutritional controversies, our editorial team, and our medical review board.
Should you find any inaccuracy in this guide, please email andreas@dietdoctor.com.
There is one published report of two pregnant women using a keto diet to control epilepsy. One woman had a baby with normal development, followed all the way to 12 months of age. The other woman’s baby had bilateral ear deformities of unknown cause, though her anti-seizure drug dose did need to be increased a total of three times during the latter two-thirds of her pregnancy.
Seizure 2017: Ketogenic diet therapy for epilepsy during pregnancy: A case series [case series report; very weak evidence] ↩
Rodent studies report that the ketogenic diet may increase or decrease the rate of growth and development of multiple organs. The significance of these findings with respect to any impact on cognitive, motor, and behavioral function is unclear. One of the rodent studies found the adult offspring of mothers fed a keto diet to be hyperactive, less depressed, and less anxious.
BMC Pregnancy Childbirth. 2013: Effects of a ketogenic diet during pregnancy on embryonic growth in the mouse [animal study; very weak evidence]
Brain Behav. 2015: Gestational ketogenic diet programs brain structure and susceptibility to depression & anxiety in the adult mouse offspring [animal study; very weak evidence] ↩
- International Diabetes Federation: Gestational Diabetes [overview article; ungraded]
- International Journal of Women’s Health 2010: Gestational Diabetes: Risks, Management, and Treatment Options [overview article; ungraded]
The New England Journal of Medicine 2008: Hyperglycemia and Adverse Pregnancy Outcomes[prospective observational study with HR<2, very weak evidence] ↩
- Clinical & Investigative Medicine 1996: Carbohydrate Intolerance in Pregnancy: Incidence and Neonatal Outcomes [retrospective observational study; very weak evidence]
- Seminars in Perinatology 2015: Pregnancy As a Window to Future Health: Excessive Gestational Weight Gain and Obesity [overview article; ungraded]
- Diabetes Care 2020: 14. Management of diabetes in pregnancy: standards of medical care in diabetes — 2020 [clinical practice guideline; ungraded]
- The Journal of the American College of Nutrition 1990: Dietary manipulation as a primary treatment strategy for pregnancies complicated by diabetes [overview article; ungraded]
- Diabetes Spectrum 2016: Carbohydrate Content in the GDM Diet: Two Views: View 1: Nutrition Therapy in Gestational Diabetes: The Case for Complex Carbohydrates [overview article; ungraded] (60% carbs)
- Diabetes Spectrum 2016: Carbohydrate Content in the GDM Diet: Two Views: View 2: Low-Carbohydrate Diets Should Remain the Initial Therapy for Gestational Diabetes [overview article; ungraded](40% carbs)
This is based on the consistent clinical experience of low-carb practitioners. [weak evidence] ↩
We are not aware of any clinical trials in pregnant women that examined a very low-carb or ketogenic diet compared to other dietary patterns. Therefore, in the absence of clinical data, much of the information presented in this guide is based on clinical experience and the extrapolation of data from non-pregnant women.
However, one trial evaluated a target intake of 130 grams of carbs (versus 200 grams) and found no harmful effects and no evidence of ketones in the blood. Unfortunately, the lower-carb group consumed an average 165 grams, with only 20% of the group meeting the 130 gram target.
American Journal of Clinical Nutrition 2020: Effects of a modestly lower carbohydrate diet in gestational diabetes: a randomized controlled trial [randomized trial; moderate evidence]
↩As of Sunday, July 23, 2017 ↩
Although Natalie tested negative for GD, it’s important to note that people on low-carbohydrate diets are prone to false positive results when they undergo an oral glucose tolerance test (OGTT). For this reason, women on low-carb diets who need to be screened for GD should consider raising their daily carbohydrate intake to above 150 grams for a minimum of three days preceding an OGTT, although at least one study suggests it may take more than a week to fully acclimate.
Diabetes 1979: Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. National Diabetes Data Group [overview article; ungraded]
Diabetes care 2022:
Prolonged glycemic adaptation following transition from a low- to high-carbohydrate diet: A randomized controlled feeding trial[moderate evidence] ↩Diabetes Care 2020: 14. Management of diabetes in pregnancy: standards of medical care in diabetes — 2020 [clinical practice guideline; ungraded] ↩
This is based on Dr. Jovanovic’s and Ms. Nichols’ clinical experience with carb restriction during pregnancy. ↩
However, we need to also acknowledge that there are no quality studies demonstrating the safety of very low carbohydrate consumption during pregnancy. Clinicians need to draw their own conclusions from the minimal evidence that does exist and their own clinical experience. ↩
This is based on Dr. Fox’s clinical experience. [anecdotal report; very weak evidence]
It is also substantiated by normal physiology seen in non-pregnant individuals in whom nutritional ketosis is safe and distinctly different than ketoacidosis. You can read more in our guide on ketosis.
↩As stated in the Disclaimer at the beginning of this guide, rodent studies have suggested possible harm, while no human studies exist. We simply do not know how higher maternal ketones and/or lower maternal glucose affect the developing fetus.
Further, some physicians may worry about higher maternal levels of free fatty acids increasing insulin resistance and making gestational diabetes worse. ↩
World Journal of Diabetes 2015: Gestational diabetes: A clinical update [overview article; ungraded] ↩
The American Diabetes Association 2014: An Early Pregnancy HbA1c ≥5.9% (41 mmol/mol) Is Optimal for Detecting Diabetes and Identifies Women at Increased Risk of Adverse Pregnancy Outcomes [non-controlled study; weak evidence] ↩
Journal of General Internal Medicine 2014: Pitfalls in Hemoglobin A1c Measurement: When Results may be Misleading [overview article; ungraded] ↩
This is based mostly on her opinion and clinical experience although some studies seem to support her hypothesis:
BMJ Open 2018: Pregnancy outcomes of early detected gestational diabetes: a retrospective comparison cohort study, Qatar [observational study, very weak evidence] ↩
Note that in the United States, CGMs are not approved by the FDA for pregnant women and therefore insurance will likely not cover them. The same may not be true in Europe or Canada.
Diabetes technology and Therapeutics 2017: CGM, Pregnancy, and Remote Monitoring [overview article; ungraded] ↩
This is based on consistent clinical experience of low-carb practitioners. [weak evidence] ↩
Journal of Clinical and Diagnostic Research 2014: Normal pregnancy- A state of insulin resistance [nonrandomized study, weak evidence] ↩
We report the recommended targets in the ADA guidelines. Some clinicians believe that even lower targets are appropriate.
Diabetes Care 2020: 14. Management of diabetes in pregnancy: standards of medical care in diabetes — 2020 [clinical practice guideline; ungraded] ↩
Although the following reference is not specific to pregnancy, clinical experience suggests that the risk of a false positive likely applies in pregnancy, as well.
Diabetes 1979: Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. National Diabetes Data Group [overview article; ungraded]
Diabetes care 2022:
Prolonged glycemic adaptation following transition from a low- to high-carbohydrate diet: A randomized controlled feeding trial[moderate evidence] ↩- An International Journal of Obstetrics & Gynaecology 2012: Glucose Challenge Test for Detecting Gestational Diabetes Mellitus: A Systematic Review [systematic review of randomized trials; strong evidence]
- American Journal of Obstetrics & Gynecology 1999: Jelly Beans As an Alternative to a Fifty-Gram Glucose Beverage for Gestational Diabetes Screening [randomized trial; moderate evidence]
- American Journal of Obstetrics & Gynecology 2015: Candy Twists As an Alternative to the Glucola Beverage in Gestational Diabetes Mellitus Screening [randomized trial; moderate evidence]
American Journal of Obstetrics & Gynecology 2016: Single Abnormal Value on 3-Hour Oral Glucose Tolerance Test During Pregnancy Is Associated with Adverse Maternal and Neonatal Outcomes: A Systematic Review and Metaanalysis [systematic review of observational studies; very weak evidence] ↩
Although this test has repeatedly been shown to diagnose more cases of GD (compared to the two-step process usually used in the US), a 2021 randomized controlled trial shows that it does not improve pregnancy-related outcomes compared to the two-step process. Therefore, the two-step process seems more favorable, as the 50-gram challenge does not need to be done fasting and the two-step process is less likely to diagnose GD in women who will not benefit from the intensive management of GD.
New England Journal of Medicine 2021: A pragmatic, randomized clinical trial of gestational diabetes screening [moderate evidence]
American Journal of Obstetrics & Gynecology 2015: The Impact of Adoption of the International Association of Diabetes in Pregnancy Study Group Criteria for the Screening and Diagnosis of Gestational Diabetes [non-controlled study; weak evidence] ↩
This strategy is not officially endorsed by medical societies but represents the opinion of the experts interviewed.
World Journal of Diabetes 2015: Indicators of Glycemic Control in Patients with Gestational Diabetes Mellitus and Pregnant Women with Diabetes Mellitus [overview article; ungraded] ↩
This is based on her clinical experience ↩